Pediatric Oncology Nurses’ Experiences With Prognosis-Related Communication
Objectives: To examine nurses’ experiences of prognosis-related communication (PRC) with parents of children with cancer.
Sample & Setting: Cross-sectional, correlational study in the pediatric oncology setting involving 316 members of the Association of Pediatric Hematology/Oncology Nurses.
Methods & Variables: Online survey regarding individual nurse factors, PRC, interprofessional collaboration, moral distress, and perceived quality of care.
Results: Nurses strongly agreed that prognostic disclosure is critical for decision making, but they are challenged in determining their role. Nurses with more years of experience and training in PRC, those working in an outpatient setting, and those with higher levels of nurse–physician collaboration reported more positive experiences with PRC. Positive experiences with PRC and collaboration were significantly associated with higher nurse-perceived quality of care and reduced nurse moral distress.
Implications for Nursing: Nurses should work to be active participants in the process of PRC by collaborating with physician colleagues. When nurses sense that prognostic discussions have been absent or unclear, they should feel confident in approaching physician colleagues to ensure parent understanding and satisfaction with communication.
Jump to a section
Healthcare providers specializing in pediatric oncology are faced with the challenge of communicating with children and their parents about the devastating news of a cancer diagnosis and its associated prognosis (Mack, Wolfe, Grier, Cleary, & Weeks, 2006). Prognostic information incorporates the revelation of the likelihood of a cure, how long the child is anticipated to live, and the kind of life the child is expected to have (Mack et al., 2006). This type of communication is referred to as prognosis-related communication (PRC).
PRC enhances decision making of patients and parents, reduces uncertainty, engenders hope, and empowers patients to live their lives (Butow, Dowsett, Hagerty, & Tattersall, 2002; Lamont & Christakis, 2003; Mack & Joffe, 2014). Lack of prognostic disclosure can result in stress, frustration, and uncertainty among patients and families (Innes & Payne, 2009). Forgoing prognosis-related discussions can lead to false optimism and significant discrepancies between patient and physician estimates of survival. Such discrepancies may prompt patients and families to pursue futile care that may negatively affect quality of life, delay referral for palliative care services, and limit end-of-life care planning (Hancock et al., 2007; Innes & Payne, 2009). Finally, lack of disclosure can leave patients and families feeling abandoned by their providers, mistrustful of their healthcare team, and less hopeful (Innes & Payne, 2009; Mack et al., 2007).
Disclosure of prognosis-related information is a process that involves numerous conversations among patients, families, and healthcare providers. The initial disclosure of prognostic information generally is considered the purview of a physician (Dewar, 2000). Patients and family members may have limited recall of what was presented during such discussions and then turn to the nursing staff for clarification of the information presented (Dewar, 2000; Rassin, Levy, Schwartz, & Silner, 2006). If what has been discussed is unclear to the nurse, the nurse may limit communication (Helft, Chamness, Terry, & Uhrich, 2011). Inadequate communication may lead a nurse to feel constrained in taking appropriate actions (Hamric & Blackhall, 2007), resulting in moral distress (Tobin, 2012). Repeated exposure to experiences of moral distress increases the risk of burnout, withdrawal from moral dimensions of patient care, and intention to leave the nursing field (Hamric, Borchers, & Epstein, 2012; Rushton, Batcheller, Schroeder, & Donohue, 2015). Pediatric oncology nurses and physicians have described the importance of team and communication in reducing exposure to moral distress (Pye, 2013).
Interprofessional collaboration is a critical aspect of teams who care for children with cancer. Collaboration enhances communication with patients and parents, supports decision making, minimizes distress, and optimizes quality of life (Wiener, Kazak, Noll, Patenaude, & Kupst, 2015). Nurse perceptions of enhanced nurse–physician collaboration have been associated with reduced risk of negative patient outcomes (Baggs et al., 1999), higher physician and nurse satisfaction with patient care quality, and reduced levels of moral distress (Hamric & Blackhall, 2007). At times, nurses caring for patients with life-limiting illnesses report a lack of collaboration with their physician colleagues regarding PRC (Reinke, Shannon, Engelberg, Young, & Curtis, 2010). When nurses are excluded from PRC with patients and their families, they may feel caught in the middle as they aim to advocate for their patients while supporting the medical team (McLennon, Uhrich, Lasiter, Chamness, & Helft, 2013).
Research targeting PRC in the pediatric oncology population is limited, and nurses’ experiences with the process are glaringly absent. The pediatric context is unique in that parents serve as the primary recipients of PRC, adding a different dynamic to the communication. The current study aimed to address this gap by exploring factors associated with pediatric oncology nurses’ experiences with PRC and the potential relationship to care they provide to patients and their parents. The specific aims were as follows:
• Examine nurses’ experiences with PRC with parents of children with cancer.
• Determine associations among individual nurse factors, nurse perceptions of PRC, and interprofessional collaboration.
• Determine if individual nurse factors, nurse perceptions of PRC, and interprofessional collaboration are associated with nurse-perceived quality of care and moral distress in the context of provider–parent communication regarding prognosis.
The Quality-Caring Model created by Duffy and Hoskins (2003) provided the conceptual foundation for the proposed research. This model aims to unveil the impact of caring nursing processes on outcomes within the complex healthcare environment. The three major components of the model are structure/causal past, process/caring relationships (independent and collaborative), and outcomes/future. Each of these components is represented in the study and operationalized as study variables, as presented in Table 1. 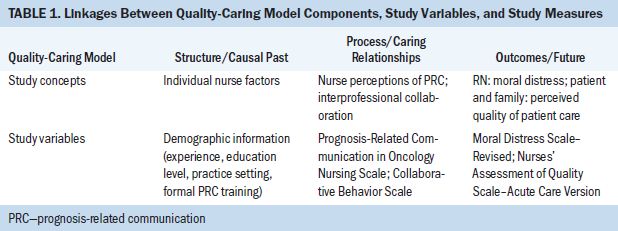
Methods
Design
A cross-sectional, correlational design was used to explore pediatric oncology nurses’ experiences with PRC with parents of children with cancer. Participants responded to an email request for participation and completed an online survey that included all study instruments.
Hypotheses
Hypotheses displayed in the study model include the following:
• Individual nurse factors (more years of experience in pediatric oncology, a master’s degree or higher, practicing in an outpatient setting, and previous formal training in PRC) are associated with more positive scores on the Prognosis-Related Communication in Oncology Nursing Scale (PRCONS) (hypothesis 1) and Collaborative Behavior Scale (CBS)–Part A (RN–physician communication) (hypothesis 2); PRCONS and CBS are positively correlated (hypothesis 3).
• Individual nurse factors and more positive scores on PRCONS and CBS are associated with higher levels of nurse-perceived quality of care, as measured by the Nurses’ Assessment of Quality Scale–Acute Care Version (NAQS-ACV) (hypothesis 4), and reduced levels of moral distress, as measured by the Moral Distress Scale–Revised (MDS-R) pediatric version (hypothesis 5); NAQS-ACV and MDS-R are negatively correlated (hypothesis 6).
Sample
Participants were recruited from the membership roster of the Association of Pediatric Hematology/Oncology Nurses (APHON), a national association of about 3,600 nurses and other healthcare providers. Pediatric oncology nurses who had at least one year of experience and were able to read and write English were eligible to participate.
A priori power analysis using G*Power 3 software for a regression model with a maximum of six predictors with an effect size of 0.15, significance level of 0.05, and 80% power resulted in a sample size estimate of 98 respondents. To ensure adequate power and representation from a broad national sample and for future psychometric evaluation of study instruments, a goal of 300 respondents was established. To be included in the analyses, respondents had to complete the demographic questionnaire and at least one other survey instrument.
Measures
Individual nurse factors: Individual nurse factors identified as possible predictors of process and outcome variables included years of experience in pediatric oncology nursing, level of education, practice setting, and formal training in PRC. For regression analyses, three variables were dichotomized: education (0 = diploma, associate degree, or bachelor’s degree; 1 = master’s or doctoral degree); practice setting (0 = inpatient; 1 = outpatient or inpatient and outpatient); and PRC training (0 = none or a little bit; 1 = a moderate amount or great deal).
Prognosis-Related Communication in Oncology Nursing Scale: PRCONS is designed to characterize nurses’ experiences with PRC (Newman & Helft, 2015). Originally designed to assess communication with patients, the instructions and items were modified with permission to assess communication with parents, because they are the primary recipients of prognostic information in the context of childhood cancer. Items are rated on a four-point Likert-type scale indicating level of agreement from 1 (strongly disagree) to 4 (strongly agree). The instrument contains three subscales: physician communication, RN role, and decision making. Composite and subscale scores can be generated. A Cronbach alpha coefficient of 0.75 was previously reported in an adult oncology nurse sample, with subscale reliability estimates ranging from 0.76–0.84 (Newman & Helft, 2015).
Collaborative Behavior Scale: CBS was designed to determine the extent of collaborative behaviors between nurses and physicians on a respondent’s unit (Stichler, 1989). Responses are rated on a four-point Likert-type scale, specifying the frequency of listed behaviors from 1 (rarely) to 4 (nearly always). Scores are summed for one composite score, with higher totals indicating more collaborative relationships. The instrument has exhibited robust reliability estimates when completed by nurses with different levels of education, ranging from a Cronbach alpha of 0.96 (Stichler, 1990) to 0.98 (Almost & Laschinger, 2002).
Nurses’ Assessment of Quality Scale–Acute Care Version: NAQS-ACV documents nurses’ evaluations of the process of nursing care (Lynn, McMillen, & Sidani, 2007). The instrument has three sections. The first section, nursing care and relationships between the nurse and patient, was used in the current study, as recommended when the patient is the unit of analysis rather than the nursing unit. This section contains four subscales, which are labeled as interaction, vigilance, individualization, and advocate. The scale’s wording was modified, with permission, to apply to the parents of pediatric patients with cancer. The four-point Likert-type scale was summed for a composite score. Subscale scores also were calculated. Cronbach alpha previously has been reported as ranging from 0.88–0.94 for the subscales (Lynn et al., 2007).
Moral Distress Scale–Revised: The MDS-R pediatric version measures levels of moral distress among healthcare providers (Hamric et al., 2012). Parallel versions of the instrument exist for nurses, physicians, and other healthcare providers in adult and pediatric settings. Scale items are based on moral dilemmas that present in health care. Each item is scored in terms of how often the situation arises (frequency) and how disturbing the situation is when it arises (intensity). Composite scores are calculated as the sum of item frequency multiplied by the intensity score. Cronbach alpha estimates have been reported at 0.9 for RNs in a large healthcare system (Whitehead, Herbertson, Hamric, Epstein, & Fisher, 2015) and 0.96 in a sample of Italian pediatric oncology nurses (Lazzarin, Biondi, & Di Mauro, 2012).
Data Collection
Prior to data collection, the study protocol was submitted to the institutional review board at Marquette University in Milwaukee, Wisconsin, and received an exempt determination. A survey request and fee were submitted to the national APHON office. Emails with an invitation to participate and a link to the survey, using SurveyMonkey®, then were sent to all APHON members through the APHON office. Email invitations were repeated two and six weeks later. The survey included an opening screen, which outlined the components of informed consent. If respondents were willing to participate, they clicked the “I agree” button and then obtained access to the survey. No direct identifiers were collected. The online survey included the four study instruments, used with permission, and a demographic questionnaire. At the end of the survey, respondents were offered the opportunity to receive a $5 gift card to thank them for their time. Data collection occurred from April to June 2016.
Data Analysis
All analyses were performed using IBM SPSS Statistics, version 24.0. Data obtained from the web-based survey were exported and stored in password-protected files on a password-protected computer with access limited to the investigator. Missing data were analyzed using the missing values analysis (MVA) function in SPSS to assess the extent of missing values for each item, as well as the amount of missingness within each case. Case mean substitution, using the participant’s scale or subscale mean, was used if less than 25% of the items were missing in a scale. Aim 1 was analyzed by examining composite and subscale scores from PRCONS. For aim 2, analyses of hypotheses 1–3 used multiple regression and correlation. For aim 3, analyses for hypotheses 4–6 employed hierarchical multiple regression and correlation.
Results
Of the 3,600 nurse members of APHON, 330 agreed to participate in the survey, with 316 completing a minimum of at least one survey instrument. About 84% of respondents (n = 265) completed all instruments in their entirety. MVA demonstrated that omitted responses were missing completely at random. Table 2 summarizes demographic characteristics of the sample. The vast majority of respondents (n = 306, 98%) were women, with a mean age of 44.1 years. Forty-nine percent (n = 156) of the nurses had a bachelor’s degree, and 41% (n = 129) had a master’s degree or higher. On average, nurses in the sample had worked as a nurse for 19 years and as a pediatric oncology nurse for 15.7 years (range = 1–40). Most respondents worked full-time as staff nurses (43%, n = 137), providing direct patient care in inpatient and outpatient settings. Responses came from throughout the United States. Thirty percent of nurses (n = 92) had received a moderate amount to great deal of training in PRC. 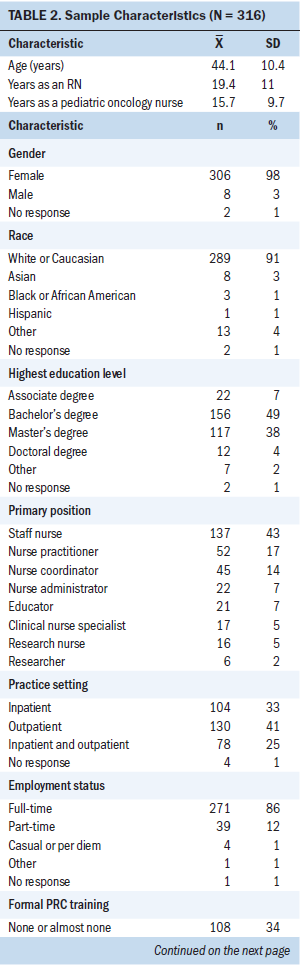
Instrument composite and subscale scores were calculated (see Table 3). Analyses for aim 1 revealed a mean composite PRCONS score that was just beyond the midpoint (52.2 on scale of 20–80), indicating positive and negative experiences with PRC. Nurses scored highest on the decision-making subscale, with an item mean of 3.2. Scores on the physician communication subscale fell just above the midpoint, with an item mean of 2.6. Lowest scores were found on the RN role subscale, with an item mean of 2.3. Mean CBS scores were in the third quartile, signifying frequent collaboration with physician colleagues. Mean total and subscale scores on the NAQS-ACV were at the higher end of the scale, with the highest scores reported on the interaction subscale. Finally, the mean composite score on the MDS-R was in the bottom quartile, indicating low levels of moral distress. The mean score on the MDS-R frequency scale also was low, but the mean score on the MDS-R intensity scale was high. 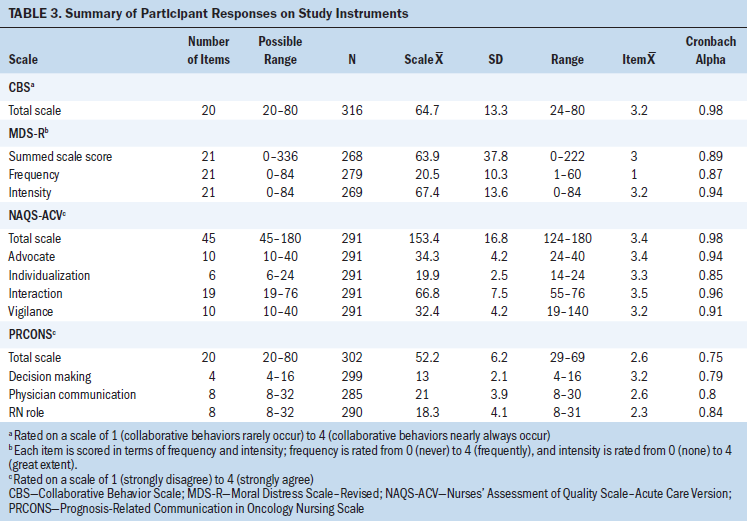
For aim 2, a regression model for the association between individual nurse factors with PRCONS (hypothesis 1) explained 17.4% of the variance in PRCONS composite scores (F[4, 294] = 15.45, p < 0.001). Three individual nurse factors were significant predictors: years of experience in pediatric oncology nursing (beta = 0.18, p = 0.002), outpatient or both inpatient and outpatient practice location (beta = 0.26, p < 0.001), and a moderate amount to great deal of training in PRC (beta = 0.14, p = 0.01).
The regression model for the association of individual nurse factors with CBS (hypothesis 2) explained 8.1% of the variance in CBS composite scores (F[4, 305] = 6.73, p < 0.001). Two individual nurse factors were significant predictors: outpatient or both inpatient and outpatient practice location (beta = 0.15, p = 0.008) and a moderate amount to great deal of previous training in PRC (beta = 0.12, p = 0.04). Figure 1 presents the summary model of relationships among study variables. 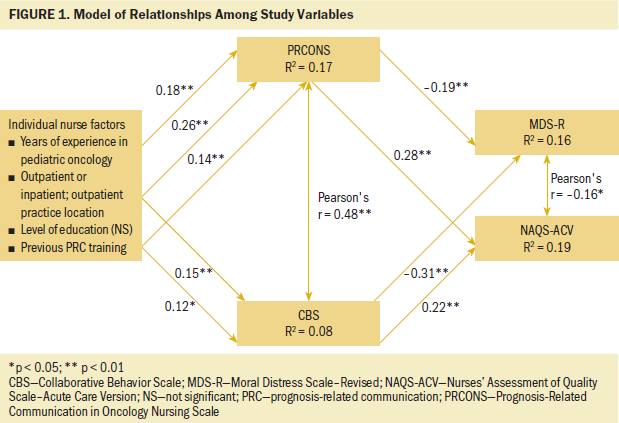
Composite scores on PRCONS and CBS were positively correlated (hypothesis 3) (r = 0.48, p < 0.001); nurses reporting more positive experiences with PRC also reported more collaborative relationships with physicians. The strongest correlation existed between the physician communication subscale and CBS (r = 0.52, p < 0.001). The RN role subscale also was significantly correlated with CBS score (r = 0.25, p < 0.001).
For aim 3, hierarchical regression analysis assessed the association of individual nurse factors, PRCONS and CBS with NAQS-ACV (hypothesis 4). Individual nurse factors were entered as step 1 and PRCONS and CBS in step 2 (see Table 4). Previous training in PRC was the only individual nurse factor found to be predictive in the initial step of the model (beta = 0.13, p < 0.05). In the final model, the total variance explained by the model was 18.7% (F[6, 278] = 10.69, p < 0.001). Nurse factors, specifically previous training in PRC, explained only 3% of the total variance in NAQS-ACV scores. Only two predictors were statistically significant in the final model: PRCONS (beta = 0.28, p < 0.001) and CBS (beta = 0.23, p < 0.001). 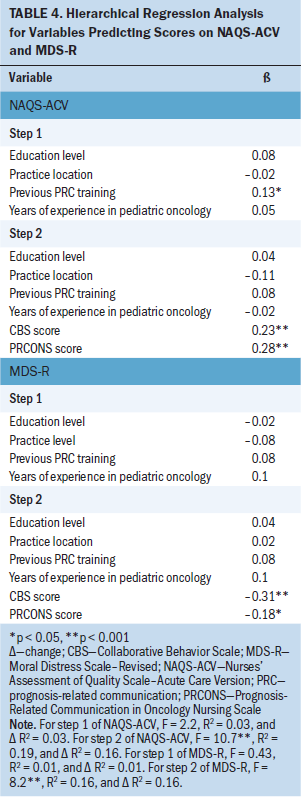
The same hierarchical regression approach was used to examine MDS-R as the outcome variable (hypothesis 5). None of the individual nurse factors entered at step 1 significantly predicted MDS-R. The total variance explained by the model as a whole was 16.1% (F[6, 258] = 8.24, p < 0.001). As with the final model predicting NAQS-ACV, CBS (beta = –0.31, p < 0.001) and PRCONS (beta = –0.19, p = 0.01) were significant predictors.
Finally, the relationship between NAQS-ACV and MDS-R composite scores was explored (hypothesis 6). A small but significant negative correlation was found between the two variables (r = –0.16, n = 266, p = 0.01), indicating an inverse relationship between perceptions of care quality and nurse moral distress.
Discussion
Descriptive analyses of PRCONS and subscale scores point to the importance that nurses place on PRC in decision making, but they suggest mixed perceptions of physician communication and challenges in determining the nurse’s role in the process. Nurses agreed that PRC is critical to decision making, which is consistent with the sentiments of parents of children with relapsed or refractory cancer (Nyborn, Olcese, Nickerson, & Mack, 2016). Results indicate that, although nurses believe that their physician colleagues are generally skilled at these conversations, they often do not occur early enough in the disease process, and nurses are not always informed when such critical conversations occur.
Nurses scored lowest on the RN role subscale of PRCONS, indicating lack of comfort and, at times, unwillingness to discuss prognosis-related concerns with parents. Similar to other studies, nurses strongly agreed that prognostic disclosure is the responsibility of the physician (Hjelmfors, Strömberg, Friedrichsen, Mårtensson, & Jaarsma, 2014; Huang et al., 2014; Schmidt Rio-Valle et al., 2009). Most nurses agreed that answering questions regarding prognosis-related information was within their scope of practice but, despite this, reported feeling uncomfortable providing life expectancy estimates if asked and did not believe that discussing estimated life expectancy was the nurse’s role. This discordance also has been documented among adult oncology and critical care nurses (Anderson et al., 2016; Helft et al., 2011).
Results suggest an opportunity for focused training in PRC to enhance communication and collaboration. Nurses who had more training reported better experiences and greater comfort with PRC. These findings are echoed by Milic et al. (2015), who found that, after a workshop on PRC skills, critical care nurses reported improved understanding of their roles and responsibilities and increased skills and confidence in participating in such discussions.
From the nurse’s perspective, collaboration with physicians was identified as a critical component of PRC; many of the results and nurses’ experiences revolved around how involved they were in the process. Nurses in the current study generally viewed relationships with their physician colleagues positively, as evidenced by higher CBS scores. CBS scores also were significantly correlated with higher PRCONS scores, suggesting that more collaborative relationships result in more comfort and better experiences with PRC. When physicians are more skilled in PRC and include the nurse, interprofessional collaboration is enhanced. However, perceived hierarchies within the healthcare profession still exist, and physicians often view themselves as singular decision makers without considering the nurse’s viewpoint (Lancaster, Kolakowsky-Hayner, Kovacich, & Greer-Williams, 2015). Such an approach creates barriers to optimal PRC. Differing definitions of collaboration between nurses and physicians, stemming from differences in professional training and role perceptions, can be effectively addressed through interprofessional education strategies. Interprofessional education aims to enable students and practitioners to gain insight and understanding of others’ roles and how they can complement one another in the complex healthcare environment. Interprofessional education enables physicians and nurses to work better together as teams and have a greater impact on patients and families (Dow & Thibault, 2017).
In the current study, nurses reported the provision of high-quality nursing care to pediatric patients with cancer and their families. Consistent with reports from Djukic, Kovner, Brewer, Fatehi, and Cline (2013) and Ryan et al. (2017), communication and collaboration were identified as playing key roles in care quality. Perceived inability to provide quality care can have a negative impact on the patient and the nurse (Williams, 1998). The perception of poor care quality can leave nurses feeling dissatisfied and stressed, which can result in frustration and guilt. Such feelings can limit the nurse’s ability to provide therapeutically effective care. Repeated inability to provide a desired level of care can result in moral distress.
Nurses in the current study sample infrequently experienced morally distressing situations. When they did, the situations themselves tended to be moderately to greatly distressing. Nurses were most distressed when they were unable to provide the high-quality compassionate care they believed the child and family required, as evidenced by a negative correlation between NAQS-ACV and MDS-R. A negative relationship also was found for MDS-R with PRCONS and CBS; improved experiences of PRC and higher levels of nurse–physician collaboration were associated with lower levels of nurse moral distress. Improving communication and collaboration appears to have the ability to minimize moral distress among pediatric oncology nurses. Conversely, lack of communication and collaboration can be distressing and can result in emotional exhaustion and depersonalizing interactions with patients, both of which are components of burnout syndrome (Allen et al., 2013; Oh & Gastmans, 2015) and compassion fatigue (Branch & Klinkenberg, 2015). Like the perception of poor quality care, moral distress can leave nurses feeling angry and frustrated, limiting their ability to cope with the challenges of oncology nursing practice. This inability to cope leads some nurses to consider leaving their job or the nursing profession altogether.
Limitations
Generalizability is limited because of the homogeneity of the sample. Although the sample is representative of nurses from across the United States, respondents were members of a professional organization and 30% (n = 92) had previous training in PRC. Also, the response rate was less than that of a similar study with adult oncology nurses (Helft et al., 2011). The reason for the low response rate in the current study is unknown.
Although the study instruments had prior evidence supporting reliability and validity, several, particularly PRCONS and NAQS-ACV, have been used in a limited fashion and not with pediatric oncology nurses. Instructions and items on PRCONS and NAQS-ACV were revised to be consistent with the population under investigation. In addition, generation of a composite score on the first section of NAQS-ACV has not been previously reported. Despite this, both instruments demonstrated good reliability with the current sample.
All instruments captured the perceptions of nurses’ experiences and, therefore, may not be reflective of observable behaviors. PRC is a process experienced by patients, family members, physicians, and other healthcare team members. The current study represents only one perspective. In addition, the current study does not link directly to patient and parent outcomes but uses the nurse’s perception of quality as a surrogate. Finally, as a cross-sectional design, the results of the current study do not infer causality.
Implications for Nursing
The current study findings suggest that nurses have the opportunity to be more actively involved in PRC, seeking out their physician colleagues to identify when critical conversations will take place. Nurses can request clarification of prognostic information when needed and indicate an interest in participating in prognostic-related discussions. Following such discussions, nurses can aim to support patients and families by determining their understanding of the information presented and recognizing when confusion or conflict may be present. Nurses with more experience with PRC should actively model these behaviors for less experienced nurses.
Nursing leaders, advanced practice providers, and educators should advocate for more interprofessional dialogue and education with their physician colleagues regarding this topic. Nurses and physicians need a better understanding of the others’ experiences and expectations to ensure optimal patient and family outcomes. Forging such discussions will be novel, time-consuming, and likely challenging, but necessary to enhance team performance. In addition, mechanisms for documenting prognostic conversations, including patient and family responses, must be identified to facilitate seamless care across the continuum.
Additional research should aim to develop and test strategies to enhance communication and interprofessional collaboration. First steps include examining the views of physicians and parents regarding nurses’ role in the process of PRC and how, through this process, nurses can improve targeted patient and family outcomes. The impact of interprofessional education focused on PRC should be explored in an effort to improve collaboration, enhance quality of care, and reduce distress among staff. Empowering nurses to engage more fully and confidently in the process of PRC, as well as nurse–physician collaboration, has the potential to contribute to improved healthcare team performance, resulting in improved quality of care and patient and family outcomes. Finally, additional research should aim to further establish the validity and reliability of study instruments for use in the pediatric oncology population. 
Conclusion
As frontline caregivers, nurses are intimately involved with PRC. Nurses often are unsure of their role and uncomfortable with some of the questions asked during these conversations with patients and families. More years of experience in pediatric oncology, training in PRC, outpatient practice setting experience, and interprofessional collaboration with physician colleagues are all associated with better experiences with the process. When interprofessional collaboration is poor or past experiences with PRC are viewed negatively, quality of care can be compromised and moral distress may develop. Pediatric oncology nurses should aim to be more active participants in the process and engage their physician colleagues to collaborate. Nurses with more years of experience can serve as mentors and role models to novice nurses in regard to nurse–physician collaboration and PRC. As providers who spend the most time with patients and families, pediatric oncology nurses must be empowered to participate in PRC in a meaningful way to ensure optimal patient and family outcomes and team functioning. 
About the Author(s)
Amy R. Newman, PhD, RN, CPNP-PC, CPHON®, is a postdoctoral fellow in the College of Nursing at the University of Utah in Salt Lake City and a pediatric nurse practitioner at the Medical College of Wisconsin in Milwaukee; Margaret Faut Callahan, CRNA, PhD, FNAP, FAAN, is the provost of the Health Sciences Division at Loyola University Chicago in Maywood, IL; Stacee M. Lerret, PhD, RN, CPNP-AC/PC, CCTC, FAAN, is an assistant professor at the Medical College of Wisconsin; and Debra L. Oswald, PhD, is a professor in the Department of Psychology, and Marianne E. Weiss, DNSc, RN, is a professor in the College of Nursing, both at Marquette University in Milwaukee, WI. This research was funded by a mentored nurse researcher grant from the Alex’s Lemonade Stand Foundation. Research reported in this publication was supported by National Institute of Nursing Research of the National Institutes of Health under award number T32NR013456 (m-PIs: Ellington and Mooney). During the writing of this article, Weiss was supported by funding from the American Nurses Credentialing Center. Newman, Callahan, Lerret, and Weiss contributed to the conceptualization and design and the manuscript preparation. Newman completed the data collection. Newman and Oswald provided statistical support. Newman and Weiss provided the analysis. Newman can be reached at amy.newman@utah.edu, with copy to ONFEditor@ons.org. (Submitted April 2017. Accepted November 14, 2017.)
References
Allen, R., Judkins-Cohn, T., deVelasco, R., Forges, E., Lee, R., Clark, L., & Procunier, M. (2013). Moral distress among healthcare professionals at a health system. JONA’S Healthcare Law, Ethics and Regulation, 15, 111–118. https://doi.org/10.1097/NHL.0b013e3182a1bf33
Almost, J., & Laschinger, H.K. (2002). Workplace empowerment, collaborative work relationships, and job strain in nurse practitioners. Journal of the American Academy of Nurse Practitioners, 14, 408–420.
Anderson, W.G., Puntillo, K., Boyle, D., Barbour, S., Turner, K., Cimino, J., . . . Pantilat, S. (2016). ICU bedside nurses’ involvement in palliative care communication: A multicenter survey. Journal of Pain and Symptom Management, 51, 589–596.
Baggs, J.G., Schmitt, M.H., Mushlin, A.I., Mitchell, P.H., Eldredge, D.H., Oakes, D., & Hutson, A.D. (1999). Association between nurse-physician collaboration and patient outcomes in three intensive care units. Critical Care Medicine, 27, 1991–1998.
Branch, C., & Klinkenberg, D. (2015). Compassion fatigue among pediatric healthcare providers. American Journal of Maternal Child Nursing, 40, 160–166.
Butow, P.N., Dowsett, S., Hagerty, R., & Tattersall, M.H. (2002). Communicating prognosis to patients with metastatic disease: What do they really want to know? Supportive Care in Cancer, 10, 161–168. https://doi.org/10.1007/s005200100290
Dewar, A. (2000). Nurses’ experiences in giving bad news to patients with spinal cord injuries. Journal of Neuroscience Nursing, 32, 324–330.
Djukic, M., Kovner, C.T., Brewer, C.S., Fatehi, F.K., & Cline, D.D. (2013). Work environment factors other than staffing associated with nurses’ ratings of patient care quality. Health Care Management Review, 38, 105–114.
Dow, A., & Thibault, G. (2017). Interprofessional education—A foundation for a new approach to health care. New England Journal of Medicine, 377, 803–805. https://doi.org/10.1056/NEJMp1705665
Duffy, J.R., & Hoskins, L.M. (2003). The Quality-Caring Model: Blending dual paradigms. Advances in Nursing Science, 26, 77–88.
Hamric, A.B., & Blackhall, L.J. (2007). Nurse-physician perspectives on the care of dying patients in intensive care units: Collaboration, moral distress, and ethical climate. Critical Care Medicine, 35, 422–429. https://doi.org/10.1097/01.CCM.0000254722.50608.2D
Hamric, A.B., Borchers, C.T., & Epstein, E.G. (2012). Development and testing of an instrument to measure moral distress in healthcare professionals. AJOB Primary Research, 3(2), 1–9.
Hancock, K., Clayton, J.M., Parker, S.M., Wal der, S. Butow, P.N., Carrick, S., . . . Tattersall, M.H. (2007). Truth-telling in discussing prognosis in advanced life-limiting illnesses: A systematic review. Palliative Medicine, 21, 507–517.
Helft, P.R., Chamness, A., Terry, C., & Uhrich, M. (2011). Oncology nurses’ attitudes toward prognosis-related communication: A pilot mailed survey of Oncology Nursing Society members. Oncology Nursing Forum, 38, 468–474. https://doi.org/10.1188/11.ONF.468-474
Hjelmfors, L., Strömberg, A., Friedrichsen, M., Mårtensson, J., & Jaarsma T. (2014). Communicating prognosis and end-of-life care to heart failure patients: A survey of heart failure nurses’ perspectives. European Journal of Cardiovascular Nursing, 13, 152–161.
Huang, S.H., Tang, F.I., Liu, C.Y., Chen, M.B., Liang, T.H., & Sheu, S.J. (2014). Truth-telling to patients’ terminal illness: What makes oncology nurses act individually? European Journal of Oncology Nursing, 18, 492–498. https://doi.org/10.1016/j.ejon.2014.04.010
Innes, S., & Payne, S. (2009). Advanced cancer patients’ prognostic information preferences: A review. Palliative Medicine, 23, 29–39.
Lamont, E.B., & Christakis, N.A. (2003). Complexities in prognostication in advanced cancer: “To help them live their lives the way they want to.” JAMA, 290, 98–104. https://doi.org/10.1001/jama.290.1.98
Lancaster, G., Kolakowsky-Hayner, S., Kovacich, J., & Greer-Williams, N. (2015). Interdisciplinary communication and collaboration among physicians, nurses, and unlicensed assistive personnel. Journal of Nursing Scholarship, 47, 275–284. https://doi.org/10.1111/jnu.12130
Lazzarin, M., Biondi, A., & Di Mauro, S. (2012). Moral distress in nurses in oncology and haematology units. Nursing Ethics, 19, 183–195. https://doi.org/10.1177/0969733011416840
Lynn, M.R., McMillen, B.J., & Sidani, S. (2007). Including the provider in the assessment of quality care: Development and testing of the Nurses’ Assessment of Quality Scale-acute care version. Journal of Nursing Care Quality, 22, 328–336. https://doi.org/10.1097/01.NCQ.0000290414.42640.c0
Mack, J.W., & Joffe, S. (2014). Communicating about prognosis: Ethical responsibilities of pediatricians and parents. Pediatrics, 133(Suppl. 1), S24–S30. https://doi.org/10.1542/peds.2013-3608E
Mack, J.W., Wolfe, J., Cook, E.F., Grier, H E., Cleary, P.D., & Weeks, J.C. (2007). Hope and prognostic disclosure. Journal of Clinical Oncology, 25, 5636–5642. https://doi.org/10.1200/JCO.2007.12.6110
Mack, J.W., Wolfe, J., Grier, H.E., Cleary, P.D., & Weeks, J.C. (2006). Communication about prognosis between parents and physicians of children with cancer: Parent preferences and the impact of prognostic information. Journal of Clinical Oncology, 24, 5265–5270. https://doi.org/10.1200/JCO.2006.06.5326
McLennon, S.M., Uhrich, M., Lasiter, S., Chamness, A.R., & Helft, P.R. (2013). Oncology nurses’ narratives about ethical dilemmas and prognosis-related communication in advanced cancer patients. Cancer Nursing, 36, 114–121.
Milic, M.M., Puntillo, K., Turner, K., Joseph, D., Peters, N., Ryan, R., . . . Anderson, W.G. (2015). Communicating with patients’ families and physicians about prognosis and goals of care. American Journal of Critical Care, 24, e56–e64.
Newman, A.R., & Helft, P.R. (2015). Reliability and validity of a tool to assess oncology nurses’ experiences with prognosis-related communication. Oncology Nursing Forum, 42, 64–73. https://doi.org/10.1188/15.ONF.64-73
Nyborn, J.A., Olcese, M., Nickerson, T., & Mack, J.W. (2016). “Don’t try to cover the sky with your hands”: Parents’ experiences with prognosis communication about their children with advanced cancer. Journal of Palliative Medicine, 19, 626–631.
Oh, Y., & Gastmans, C. (2015). Moral distress experienced by nurses: A quantitative literature review. Nursing Ethics, 22, 15–31. https://doi.org/10.1177/0969733013502803
Pye, K. (2013). Exploring moral distress in pediatric oncology; a sample of registered practitioners. Issues in Comprehensive Pediatric Nursing, 36, 248–261. https://doi.org/10.3109/01460862.2013.812693
Rassin, M., Levy, O., Schwartz, T., & Silner, D. (2006). Caregivers’ role in breaking bad news: Patients, doctors, and nurses’ points of view. Cancer Nursing, 29, 302–308.
Reinke, L.F., Shannon, S.E., Engelberg, R.A., Young, J.P., & Curtis, J.R. (2010). Supporting hope and prognostic information: Nurses’ perspectives on their role when patients have life-limiting prognoses. Journal of Pain and Symptom Management, 39, 982–992. https://doi.org/10.1016/j.jpainsymman.2009.11.315
Rushton, C.H., Batcheller, J., Schroeder, K., & Donohue, P. (2015). Burnout and resilience among nurses practicing in high-intensity settings. American Journal of Critical Care, 24, 412–420. https://doi.org/10.4037/ajcc2015291
Ryan, C., Powlesland, J., Phillips, C. Raszewski, R., Johnson, A., Banks-Enorense, K., . . . Welsh, J. (2017). Nurses’ perceptions of quality care. Journal of Nursing Care Quality, 32, 180–185.
Schmidt Rio-Valle, J., Garcia Caro, M.P., Montoya Juarez, R., Prados Peña, D., Muñoz Vinuesa, A., Pappous, A., & Cruz Quintana, F. (2009). Bad news for the patient and the family? The worst part of being a health care professional. Journal of Palliative Care, 25, 191–196.
Stichler, J.F. (1989). Development and psychometric testing of a collaborative behavior scale. Unpublished manuscript, University of San Diego, Philip Y. Hahn School of Nursing.
Stichler, J.F. (1990). The effects of collaboration, organizational climate, and job stress on job satisfaction and anticipated turnover in nursing. Ann Arbor, MI: University Microfilms, International.
Tobin, G.A. (2012). Breaking bad news: A phenomenological exploration of Irish nurses’ experiences of caring for patients when a cancer diagnosis is given in an acute care facility (part 1). Cancer Nursing, 35, E21–E29. https://doi.org/10.1097/NCC.0b013e318241921d
Whitehead, P.B., Herbertson, R.K., Hamric, A.B., Epstein, E.G., & Fisher, J.M. (2015). Moral distress among healthcare professionals: Report of an institution-wide survey. Journal of Nursing Scholarship, 47, 117–125. https://doi.org/10.1111/jnu.12115
Wiener, L., Kazak, A.E., Noll, R.B., Patenaude, A.F., & Kupst, M.J. (2015). Interdisciplinary collaboration in standards of psychosocial care. Pediatric Blood and Cancer, 62(Suppl. 5), S425. https://doi.org/10.1002/pbc.25718
Williams, A.M. (1998). The delivery of quality nursing care: A grounded theory study of the nurse’s perspective. Journal of Advanced Nursing, 27, 808–816. https://doi.org/10.1046/j.1365-2648.1998.00590.x


