Feasibility and Acceptability of Distress Screening for Family Caregivers at a Cancer Surgery Center
Objectives: To determine the feasibility and acceptability of a validated electronic distress screening program for cancer caregivers.
Sample & Setting: 17 informal caregivers presenting with a patient with cancer to an ambulatory cancer surgery center.
Methods & Variables: Caregivers completed the CancerSupportSource®—Caregiver screening and a brief semistructured interview concerning the screening.
Results: Caregivers described the screening as straightforward and comprehensive. They endorsed concerns about their self-care needs but were most likely to request information or a referral for patient-focused concerns. Referrals generated from the program are likely viably addressed with existing supportive care resources.
Implications for Nursing: Brief, caregiver-focused distress screening is perceived positively by caregivers. Caregivers indicated that they felt it validated the importance of their role and highlighted the hospital’s efforts to continually improve care. This screening program may be particularly beneficial in ambulatory surgical centers to efficiently identify caregivers with concerns and provide a point of entry to remediate these concerns.
Jump to a section
Caregiving is psychosocially demanding. However, a supportive informal caregiver provides invaluable assistance to patients, helping them adhere to and receive the most benefit from their cancer care (Kissane, 2013). The approximately 3 million Americans who were caregivers to people with cancer comprise relatives, friends, and partners who have a significant relationship with and provide assistance (e.g., physical, emotional) to the patient (National Alliance for Caregiving, 2016; National Alliance for Caregiving & AARP Public Policy Institute, 2015). As a result of these demands, caregivers are at risk for clinically significant symptoms of depression and anxiety (Braun, Mikulincer, Rydall, Walsh, & Rodin, 2007; Chambers et al., 2013; Janda et al., 2007; Sklenarova et al., 2015) and medical morbidity (Beesley, Price, & Webb, 2011; Buyck et al., 2013; Ji, Zöller, Sundquist, & Sundquist, 2012; Morris et al., 2015; Vitaliano et al., 2002). Despite the need for interventions to support caregivers and the existence of multiple programs that are successful in doing so (Northouse, Katapodi, Song, Zhang, & Mood, 2010), such services are typically underused by caregivers (Applebaum, Farran, Marziliano, Pasternak, & Breitbart, 2014). This underuse may be attributable, in part, to multiple practical and psychological barriers that interfere with caregivers’ access to services (Adam, 2000; Applebaum et al., 2014; Morris & Thomas, 2001; Ramirez, Addington-Hall, & Richards, 1998; Shaw et al., 2013). As such, procedures like routine distress screening that efficiently identify caregivers with supportive care needs and triage them to accessible interventions and resources will be critical to overcoming these barriers.
Despite repeated calls to integrate family-centered support services into cancer care (Kent et al., 2016), most adult oncology practice settings have not established standardized protocols to identify caregivers with greater emotional, social, and practical support needs. Although there is documented need (Vanderwerker, Laff, Kadan-Lottick, McColl, & Prigerson, 2005) and strong demand for psychosocial services (Applebaum et al., 2014; Baghi et al., 2007; Dionne-Odom et al., 2018; Nightingale et al., 2016), only about one in four caregivers access psychosocial care (Applebaum et al., 2014; Glasdam, Jensen, Madsen, & Rose, 1996). Distressed caregivers report higher interest in supportive interventions compared to caregivers with lower distress (Nightingale et al., 2016). Caregivers frequently cite various barriers that contribute to this notable limited uptake of services, including the following: scheduling difficulty and limited time, lack of knowledge of resources, desire not to bother the healthcare team, and belief that accessing such care would inappropriately put their needs ahead of the patients’ needs (Applebaum et al., 2014; Badr et al., 2016; Shaw et al., 2013; Waldron, Janke, Bechtel, Ramirez, & Cohen, 2013).
Among people with cancer, distress screening has been found to be an efficient way to identify individuals with high unmet needs and triage them into the appropriate level of supportive care (Carlson, Groff, Maciejewski, & Bultz, 2010), overcoming many treatment access barriers. Assessing and addressing psychosocial needs has been associated with important clinical benefits for patients, including reduced distress and fewer hospitalizations, emergency department visits, and number of filled prescriptions (Carlson et al., 2010; Sobel, 2000). The Institute of Medicine ([IOM], 2008) and the National Comprehensive Cancer Network ([NCCN], 2018) have recognized that screening, referral, and follow-up for psychosocial concerns are critical to ensuring high-quality comprehensive cancer care. However, extant distress screening programs have primarily targeted patients alone, which ignores the reality that psychosocial distress in the cancer context is frequently interrelated between patients and their families (Girgis, Lambert, Johnson, Waller, & Currow, 2013; Shaffer, Kim, & Carver, 2016).
Developing and implementing a caregiver-focused distress screening program has significant potential to improve quality of care for all those affected by cancer. Beyond addressing the substantial mental and physical health burdens experienced by caregivers, such routine procedures may begin to shift caregivers’ and healthcare systems’ cultural norms around caring for caregivers, moving this from the exception to a typical occurrence. Working toward these aims, the current authors conducted a feasibility study of CancerSupportSource®–Caregiver, a validated electronic distress screening program designed to address the unique concerns of cancer caregivers (Longacre et al., 2017; Zaleta et al., 2017). The two primary purposes of this study were (a) to characterize the concerns and preferred responses to concerns identified by caregivers at the time of their family members’ ambulatory surgery and (b) to determine the extent to which caregivers find screening at that time in the care continuum to be acceptable and feasible.
Methods
Design, Participants, and Setting
To answer primary study aims, quantitative (Caregiver Support Source–Caregiver responses) and qualitative (interview) data were collected for this mixed-methods feasibility study. Participants were primary, informal caregivers presenting to the Josie Robertson Surgery Center (JRSC) at Memorial Sloan Kettering Cancer Center in New York, New York, with their family member patient with cancer in March 2018; they were identified by convenience sampling from among the total population of presenting caregivers. JRSC is a first-of-its-kind, free-standing outpatient facility for ambulatory cancer surgery. Given the short-stay nature of procedures performed at this hospital, patients are required to present with a caregiver who is aged 18 years or older and agrees and is able to fulfill assigned responsibilities during the pre-, intra-, and postoperative phases. The only additional eligibility criterion for this study was comfort with speaking and reading English. Only one caregiver participated per patient.
Procedure
Potentially eligible caregivers were approached by the perioperative nurse liaison (C.B.) and the interviewer (K.M.S. or S.B.) during the perioperative nurse liaison’s routine rounds through the family waiting room. If the caregiver was comfortable communicating in English, the perioperative nurse liaison provided a brief introduction to the interviewer and the study. The purpose of the study was described to caregivers as follows: The hospital is interested in determining ways to better link family caregivers to available services at the hospital and at community partners, such as the Cancer Support Community (CSC), and this study is intended to assess caregivers’ opinions of the CancerSupportSource–Caregiver screening process.
No personally identifying information was collected from caregivers, and as such, this study protocol was approved for exempt status under the hospital’s institutional review board. After providing verbal agreement to participate, caregivers individually completed study procedures in a private consultation room. Caregivers first completed self-reported demographic information with paper and pencil, then completed the CancerSupportSource–Caregiver screening and a brief semistructured interview. There was no compensation for participating.
Caregiver Distress Screening
Details concerning the development and validation of CancerSupportSource–Caregiver among cancer caregivers in the CSC affiliate support network have been noted elsewhere (Longacre et al., 2017; Zaleta et al., 2017), and the program is implemented at more than 40 of the CSC’s community-based facilities. This program was based on the CSC’s CancerSupportSource–Patient, a web-based distress screening and referral program for people with cancer (Miller, Mullins, Onukwugha, Golant, & Buzaglo, 2014). These programs were developed in accordance with the IOM’s (2008) guidelines for comprehensive management of psychosocial distress in the cancer context, recognizing that diverse unmet psychosocial needs can have profound effects on the well-being of people with cancer and their families.
CancerSupportSource–Caregiver asks caregivers to rate their level of concern for 33 possible problems (see Table 1) and how they would prefer these concerns to be addressed. The screening is completed by an Internet-enabled tablet computer; data entered into the screening program are encrypted and stored in a secure, Health Insurance Portability and Accountability Act–compliant database. Responses are not forced to any item; data are missing where participants intentionally or unintentionally did not indicate a response. Because the purpose of this study was to naturalistically observe caregivers’ use of the screening program, researchers did not intervene to limit missing data. 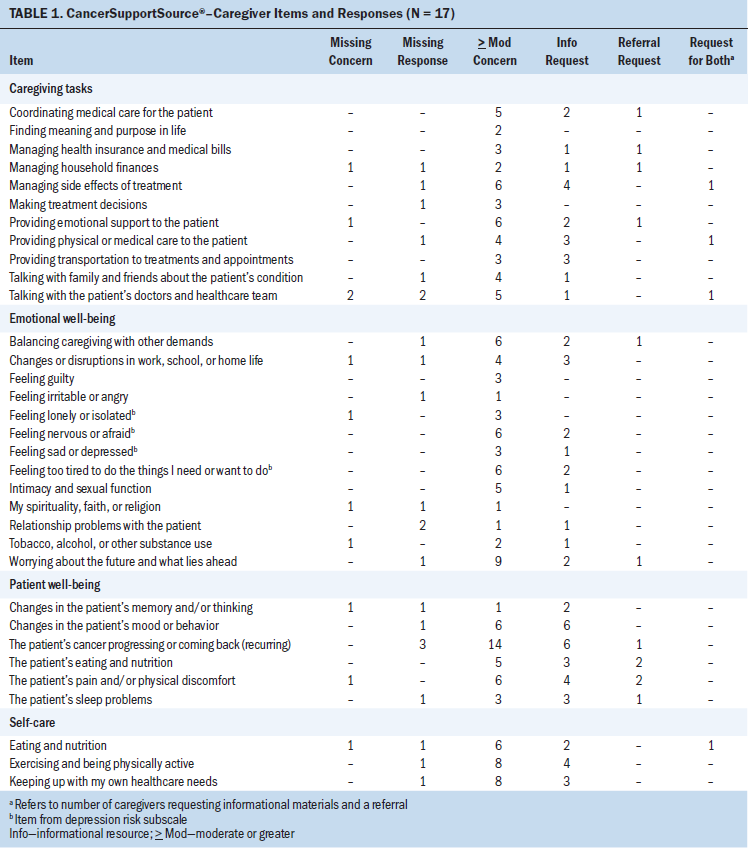
Possible concerns that were assessed included problems with caregivers’ self-care needs, emotional well-being, and caregiving tasks, and perceived concerns about the patient’s well-being. If a potential concern was rated as being of low concern (a little or not at all), caregivers were able to request pertinent educational materials (informational resource request). If a significant concern was endorsed (moderately, seriously, or very seriously), caregivers also had the option to request to speak with someone about that need (referral request) and/or receive information. A referral is not automatically generated when a caregiver endorses a significant concern for two reasons: The caregiver’s autonomy is respected when concerns are addressed according to his or her preferences, and it acknowledges that caregivers may be receiving support elsewhere for the concern. Referral sources within the hospital were designated to address each item (e.g., chaplaincy for spiritual concerns, patient financial services for fiscal concerns). Regardless of the level of concern endorsed, caregivers were able to request that no action be taken for the concern at that time. Participants who requested information about a concern were provided with relevant hard-copy materials from the hospital and the community partner at the completion of their participation; those who requested a referral were provided with the contact information of the appropriate hospital resource at the completion of their participation.
Two scores were calculated from the screening. An overall distress score was calculated by summing the level of concern across the 33 items. Each item was rated on a scale ranging from 0 (not at all) to 4 (very seriously), and total scores could range from 0 to 132, with higher scores indicating greater distress. Content validity of this total score has been established (Longacre et al., 2017). A depression risk subscale score was calculated by summing scores from four items (i.e., feeling lonely or isolated, feeling nervous or afraid, feeling sad or depressed, and feeling too tired to do the things I need or want to do), with a score of five or greater indicating risk for clinically significant depression (Buzaglo et al., 2014). For those with missing data (n = 3 for total distress score, n = 1 for depression risk score), mean imputation was used to adjust for missing responses. Participants who met criteria for depression risk were assessed for imminent self-harm and provided with a referral to the hospital’s counseling center.
Semistructured Qualitative Interviews
On completion of CancerSupportSource–Caregiver, the first five participating caregivers completed a brief interview intended to identify any significant problems with the screening or interview process; the subsequent 12 caregivers completed a brief interview regarding perceived acceptability and feasibility of the screening process. As a result, the pilot participants and the acceptability and feasibility participants completed slightly different interviews. Interviews lasted approximately 15 minutes. Semistructured interview guides were developed by K.M.S., S.B., and A.J.A. for both study phases, and interviewers used ad hoc clarifying and elaborating probes as appropriate. The two interviewers (K.M.S. and S.B.) were trained on the interview guides and had prior experience completing qualitative interviews with cancer caregivers. Interviewers had no preexisting relationships with the participants, and there was no follow-up contact between interviewers and participants. Interviewers took comprehensive notes during the interview; interviews were audio recorded to validate notes as needed, and recordings were destroyed within 48 business hours.
Analysis
Interview notes were reviewed by K.M.S. and A.J.A. using inductive thematic textual analysis, an iterative process of review, interpretation, and consensus discussions (Patton, 2002). The two coders read the field notes and identified important content independently, then shared their independent coding results and collectively generated overarching themes that emerged (Miles, Huberman, & Saldaña, 2014). Key exemplary quotations of themes were then extracted.
Results
Sample characteristics are listed in Table 2. The sample was characteristic of the population of primary caregivers presenting to the study hospital in 2017, during which time the most commonly reported relationship between the patient and the presenting primary caregiver was spouse or partner, and the median age of patients was 55 years (per internal clinic data). The mean age of caregivers in the current study was 59 years (range = 36–83). 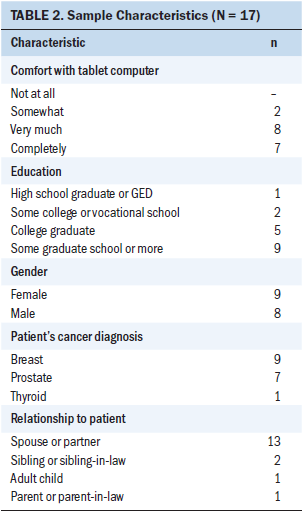
Quantitative Findings
Recruitment and screening completion: Of the 28 caregivers approached to participate, only three refused (11% refusal rate). All three who refused stated that the estimated study participation time (30–45 minutes) was too long. Eight caregivers who initially agreed to participate were not able to be enrolled because of constraints on the interviewers’ time at the hospital. As such, 17 caregivers completed the study.
On average, participant time to complete CancerSupportSource–Caregiver was 11.3 minutes (range = 6–18 minutes). Six caregivers had missing data. Of the 66 items (33 problem areas assessing level of concern and desired follow-up, if any), three individuals missed one item, two individuals missed three items, and one individual missed 25 items. Missing responses were more common for responses regarding desired follow-up (n = 23 missing responses) than for the rating of the severity of concern (n = 11).
Distress scores: Caregivers, on average, reported a distress score of 31.1 (SD = 26.8, range = 3.7–117). Five caregivers met the depression risk threshold score of five or greater. Sixteen caregivers reported that at least one item was of moderate or greater concern (median = 8, range = 1–31 items of moderate or greater concern per person). Items most commonly rated as being of moderate or greater concern were as follows:
• The patient’s cancer progressing or coming back (recurring) (n = 14)
• Worrying about the future and what lies ahead (n = 9)
• Exercising and being physically active (n = 8)
• Keeping up with my own healthcare needs (n = 8)
Requested response to concerns: Ten caregivers requested informational resources for at least one concern area (median = 7.5, range = 1–14 informational resource requests per person). Concerns for which caregivers most commonly requested informational resources were related to the following:
• Patient well-being (changes in the patient’s mood or behavior, n = 6; the patient’s cancer progressing or coming back [recurring], n = 6; the patient’s pain and/or physical discomfort, n = 4)
• Exercising and being physically active (n = 4)
• Managing symptoms or side effects of treatment (e.g., nausea, swelling) (n = 4).
Five caregivers requested at least one referral, for a total of 16 referrals generated (median = 2, range = 1–6 referrals per person). Referrals were most commonly requested in response to caregiving task concerns (n = 7) and patient well-being concerns (n = 6).
Qualitative Findings
Two key themes emerged from the qualitative interviews (see Figure 1). Caregivers described feeling as though the screening demonstrated that the hospital acknowledged and appreciated their important role in patients’ health care, and caregivers were appreciative of that recognition. In addition, caregivers described the screening as reinforcing their perception that the hospital is committed to consistently improving health care for everyone affected by cancer. Caregivers also described how the screening provided them with a unique opportunity to talk about their caregiving experience. Caregivers reported that their focus was on providing care to their family member and that the screening process helped them feel as though they were given permission to consider their own needs by being offered space to discuss their challenges as a caregiver. Several caregivers also noted that it was helpful to learn about the many supportive services available to them in the hospital and the community. 
Interviews also revealed practical considerations about screening (see Figure 2). Caregivers acknowledged that they experienced significant stress while waiting during their family member’s surgical procedure and believed that this could be a barrier to screening uptake for some caregivers. However, they felt it was an “optimal” (male acceptability and feasibility participant 1 in his 50s) and “considerate” (female acceptability and feasibility participant 10 in her 50s) time for the screening because it served as a distraction and a coping mechanism. Although most caregivers appreciated the timing of the screening, there was variability in their stated preferences for and perceived drawbacks to various times for completing screening. When directly asked about screening process concerns, no caregivers expressed concerns. Two caregivers (female acceptability and feasibility participant 7 in her 70s and male pilot participant 2 in his 70s) expressed their appreciation for knowing the confidentiality of the screening and interview data; this information was conveyed as part of the verbal consent procedure for study participation. 
Interviews also highlighted modifications that would improve the screening experience. Two caregivers (female acceptability and feasibility participant 7 in her 40s and male acceptability and feasibility participant 9 in his 30s) noted that being approached by two individuals in the waiting room while their loved one was in surgery was stressful. Two caregivers (male pilot participant 1 in his 60s and female pilot participant 4 in her 60s) noted that they would have liked clarification about the response to concerns option. Although they had significant concerns about several problem areas, they felt as though they were receiving the support they needed elsewhere. These participants selected the “nothing at this time” response, but they felt rude declining intervention from the institution. Although caregivers indicated that the screening was “simple” (female acceptability and feasibility participant 3 in her 60s), “user-friendly” (female acceptability and feasibility participant 10 in her 50s), and “straightforward” (female acceptability and feasibility participant in her 40s), some caregivers indicated their difficulty with quantifying responses to the questions. One caregiver (female acceptability and feasibility participant 2 in her 70s) stated that the answer categories were too broad for her to understand: “Slightly/moderately . . . what’s the difference? Questions like managing your loved one’s care [are] broad too. There’s so much that goes into that.” Another caregiver (female pilot participant 4 in her 60s) said she had difficulty responding when questions did not feel applicable: “[The screening was] mostly easy enough [but] would be easier if [patient’s name] was my spouse or my child or we lived together. . . . A couple of questions were difficult because we’re siblings and not living together.” One caregiver (female acceptability and feasibility participant 7) suggested adding an instructions page to introduce the screening, which could be helpful in preempting some of the noted concerns.
Discussion
This study presents evidence of the acceptance, utility, and feasibility of electronic distress screening among caregivers at the time of their family members’ ambulatory surgery. Caregivers generally described the screening as straightforward and comprehensive. Important modifications to the screening process (e.g., adding an instructions page) and study procedure (e.g., approach by one study member) were suggested. Participants perceived the screening as a validation of the importance and challenge of their role in patients’ health care, as well as emblematic of the hospital’s mission to continually improve health care for all those affected by cancer. Only 5 of 17 caregivers requested to speak with someone about a concern, and no service generated more than two referrals, suggesting that supportive care services would not be overwhelmed by full-scale implementation of such a program. Although additional study is warranted to understand how this program might ultimately improve caregivers’ well-being and help them to overcome common treatment uptake barriers, preliminary evidence showing that this program is well received by caregivers and feasible at the patients’ point of care is promising.
Caregivers frequently rated their own self-care needs as significant concerns, but they were most likely to request information or a referral for concerns related to the patients’ well-being. Prior validation studies among caregivers at community cancer support centers found contrasting findings: Although caregivers frequently rated patient well-being issues as significant concerns, they more often requested to speak with someone about their own emotional well-being concerns (Longacre et al., 2017). Caregivers in the current study had some significant personal self-care concerns, but they believed that many of these matters were already being addressed elsewhere, such as by their primary care physician. Findings may reflect the differing contexts where screening occurs: the patients’ cancer hospital as the optimal resource to address patient-related concerns versus community support organizations and caregivers’ own healthcare providers as optimal resources to address caregivers’ personal concerns. Matching caregivers’ needs to organizations most suited to providing appropriate services will be important to ensure that caregivers’ needs are met in the context of already overburdened healthcare systems. However, several caregivers in the current study were surprised to learn how many resources were available to them at the hospital, suggesting the utility of such a distress screening program to link caregivers directly with available resources targeted to their needs. In addition, this program may have even greater utility within contexts serving populations with more limited access to healthcare services, who may have no other providers to address their personal emotional and self-care needs.
Findings from the current study also quelled a concern faced by the study team prior to completing the feasibility study: that caregivers would generally be unwilling or unable to complete the screening because of distress. Caregivers agreed to participate in this study at a notably higher rate (25 agreed of 28 approached) than is typical among cancer caregiver research studies (53%–58%) (Kent et al., 2016). Participants reported a broad range of distress levels. Caregivers also described how other caregivers might be too overwhelmed to complete screening in the waiting room; however, they found the screening to be a helpful distraction and coping tool for managing their distress at that time. Although caregivers generally described the waiting period as a good time to complete the screening because it was devoid of caregiving responsibilities, there was some variability noted in caregivers’ preferred time to complete screening. The perioperative period may be an optimal time for most caregivers to complete screening, but investigating other options for screening delivery to accommodate caregivers’ differing preferences will be important for ensuring broad uptake of the screening.
Limitations and Future Research
Three primary factors limit the findings from this study. Qualitative interviews were brief; therefore, the themes identified regarding screening feasibility and acceptability during the perioperative period may not be exhaustive. In addition, the interviews were not transcribed, and the authors did not use qualitative analytics software to evaluate the narratives. Brief interviews were used for two primary reasons: (a) to limit caregivers’ participation burden during the distressing perioperative time and (b) to increase the number of caregivers able to participate per day, given the limited window each morning when procedures are conducted. Despite these design considerations, the authors were unable to enroll eight eligible and potentially interested caregivers because of the limited amount of time available from study staff who donated their time to this project. Future studies will ensure that personnel support is available for all eligible and interested participants to enroll.
This study was completed at a free-standing surgical facility that serves patients eligible for outpatient procedures (e.g., lumpectomies, prostatectomies) who tend to have nonmetastatic disease, often with chance of cancer cure or long-term survival. As such, the experience of a distinct group of caregivers was captured. Future extensions of this work to inpatient surgical and outpatient care facilities, as well as to less resourced institutions, where the distress and need for psychosocial support may be greater because of caregivers’ more complicated and lengthy caregiving trajectories and patients’ poor prognoses, are needed.
Because no identifying participant data were collected, data were cross-sectional, and there were no data regarding uptake of supportive services. For the next phase of research, the research team will complete a small-scale randomized controlled trial comparing the CancerSupportSource–Caregiver distress screening program with automated referrals to enhanced usual care (i.e., providing caregivers access to resource lists for informational guides and services available at the hospital). Findings are potentially significant in that (a) a procedure that effectively connects caregivers to resources will substantively increase the reach of existing, efficacious caregiver interventions that have been underused and narrowly disseminated and (b) by identifying specific needs and tailoring referrals to those needs, this system may help to optimize healthcare provided to caregivers, ultimately reducing service wait times and healthcare costs and increasing health systems’ responsiveness to caregivers’ needs.
Implications for Practice
Nursing care is increasingly focused on patients and families. Recognizing the important role that caregivers play in surgical recovery supports optimized care in a healthier home environment. Many caregivers perform tasks at home that are similar to those performed by professional nursing staff (National Alliance for Caregiving, 2016; National Alliance for Caregiving & AARP Public Policy Institute, 2015). This is the case at the hospital in the current study; almost all the patients undergoing prostate or breast surgery are discharged to their homes with a catheter or drain with which the caregiver must demonstrate maintenance competency prior to patient discharge. Short-stay and ambulatory surgical centers may benefit from such a measure to routinely identify caregivers with concerns about their care requirements and provide a point of entry to discuss and remediate these concerns. Supporting caregivers promotes the delivery of quality care throughout the patient’s recovery and beyond.
Beyond concerns about caregiving responsibilities, caregivers in this study appreciated the opportunity to identify, share, and address needs related to their own well-being, as well as those of their family members with cancer. In lieu of formal assessment, practitioners can greatly benefit caregivers by acknowledging that caregiving can be challenging, reinforcing that caring for themselves is essential, and providing a list of key informational and supportive care resources available to them (Porter & Dionne-Odom, 2017). Implementing extant validated screening procedures, such as CancerSupportSource–Caregiver, would help to better ensure that all caregivers’ needs are routinely and comprehensively assessed and addressed.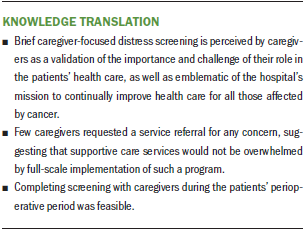 
Conclusion
Routine, comprehensive, and confidential distress screening via CancerSupportSource–Caregiver was acceptable to and appreciated by caregivers who had a family member undergoing ambulatory surgery. Issues most frequently rated as being of significant concern to caregivers did not tend to align with the issues for which caregivers requested information or referrals, which may reflect caregivers meeting their needs in other healthcare settings or a perception that oncology centers exclusively address needs of individuals with cancer. Caregivers were frequently interested in informational resources, and few referrals were generated, suggesting a modest increase in referrals that may be viably addressed with existing resources. Additional study will help to determine whether such a system that efficiently routes caregivers to the information and resources matching their needs and preferences may improve caregiving burden and caregivers’ overall quality of life. 
About the Author(s)
Kelly M. Shaffer, PhD, is a postdoctoral fellow, and Stephanie Benvengo, MA, is a research study assistant, both in the Department of Psychiatry and Behavioral Sciences at Memorial Sloan Kettering Cancer Center in New York, NY; Alexandra K. Zaleta, PhD, is a senior director of research in the Research and Training Institute at the Cancer Support Community in Philadelphia, PA; Marcia Levine, MSN, RN, NE-BC, is a senior director of perioperative services, Courtney Bellantoni, MPA, BSN, RN, OCN®, is a perioperative nurse liaison, and Aimee Dannaoui, MSN, RN, CAPA, is a nurse leader, all in the Josie Robertson Surgery Center at Memorial Sloan Kettering Cancer Center; Joanne S. Buzaglo, PhD, is the executive director of PRO solutions at Vector Oncology in Memphis, TN; and Allison J. Applebaum, PhD, is an assistant attending psychologist in the Department of Psychiatry and Behavioral Sciences at Memorial Sloan Kettering Cancer Center. This research was funded, in part, by a cancer center support grant (P30 CA008748) from the National Institutes of Health National Cancer Center. During the writing of this article, Shaffer was supported by a grant (T32 CA009461) from the National Institutes of Health National Cancer Center. Buzaglo has previously consulted for Carevive and is employed by Vector Oncology. Shaffer, Zaleta, Levine, Bellantoni, Dannaoui, Buzaglo, and Applebaum contributed to the conceptualization and design. Shaffer, Benvengo, Levine, Bellantoni, and Dannaoui completed the data collection. Shaffer and Applebaum provided statistical support and the analysis. All authors contributed to the manuscript preparation. Shaffer can be reached at kshaffer@virginia.edu, with copy to ONFEditor@ons.org. (Submitted June 2018. Accepted August 20, 2018.)
References
Adam, J. (2000). Discharge planning of terminally ill patients home from an acute hospital. International Journal of Palliative Nursing, 6, 338–345. https://doi.org/10.12968/ijpn.2000.6.7.12647
Applebaum, A.J., Farran, C.J., Marziliano, A.M., Pasternak, A.R., & Breitbart, W. (2014). Preliminary study of themes of meaning and psychosocial service use among informal cancer caregivers. Palliative and Supportive Care, 12, 139–148. https://doi.org/10.1017/S1478951513000084
Badr, H., Herbert, K., Reckson, B., Rainey, H., Sallam, A., & Gupta, V. (2016). Unmet needs and relationship challenges of head and neck cancer patients and their spouses. Journal of Psychosocial Oncology, 34, 336–346. https://doi.org/10.1080/07347332.2016.1195901
Baghi, M., Wagenblast, J., Hambek, M., Radeloff, A., Gstoettner, W., Scherzed, A., . . . Knecht, R. (2007). Demands on caring relatives of head and neck cancer patients. Laryngoscope, 117, 712–716. https://doi.org/10.1097/MLG.0b013e318031d0b4
Beesley, V.L., Price, M.A., & Webb, P.M. (2011). Loss of lifestyle: Health behaviour and weight changes after becoming a caregiver of a family member diagnosed with ovarian cancer. Supportive Care in Cancer, 19, 1949–1956. https://doi.org/10.1007/s00520-010-1035-2
Braun, M., Mikulincer, M., Rydall, A., Walsh, A., & Rodin, G. (2007). Hidden morbidity in cancer: Spouse caregivers. Journal of Clinical Oncology, 25, 4829–4834. https://doi.org/10.1200/JCO.2006.10.0909
Buyck, J.-F., Ankri, J., Dugravot, A., Bonnaud, S., Nabi, H., Kivimäki, M., & Singh-Manoux, A. (2013). Informal caregiving and the risk for coronary heart disease: The Whitehall II study. Journals of Gerontology Series A, 68, 1316–1323. https://doi.org/10.1093/gerona/glt025
Buzaglo, J., Miller, M.F., Gayer, C., Morris, A., Kennedy, V., & Golant, M. (2014). CancerSupportSource: Validating a 13-item web-based distress screening tool in the community. Paper presented at the 19th Annual Conference of the National Comprehensive Cancer Network, Hollywood, FL.
Carlson, L.E., Groff, S.L., Maciejewski, O., & Bultz, B.D. (2010). Screening for distress in lung and breast cancer outpatients: A randomized controlled trial. Journal of Clinical Oncology, 28, 4884–4891. https://doi.org/10.1200/JCO.2009.27.3698
Chambers, S.K., Schover, L., Nielsen, L., Halford, K., Clutton, S., Gardiner, R.A., . . . Occhipinti, S. (2013). Couple distress after localised prostate cancer. Supportive Care in Cancer, 21, 2967–2976. https://doi.org/10.1007/s00520-013-1868-6
Dionne-Odom, J.N., Applebaum, A.J., Ornstein, K.A., Azuero, A., Warren, P.P., Taylor, R.A., . . . Bakitas, M.A. (2018). Participation and interest in support services among family caregivers of older adults with cancer. Psycho-Oncology, 27, 969–976. https://doi.org/10.1002/pon.4603
Girgis, A., Lambert, S., Johnson, C., Waller, A., & Currow, D. (2013). Physical, psychosocial, relationship, and economic burden of caring for people with cancer: A review. Journal of Oncology Practice, 9, 197–202. https://doi.org/10.1200/JOP.2012.000690
Glasdam, S., Jensen, A.B., Madsen, E.L., & Rose, C. (1996). Anxiety and depression in cancer patients’ spouses. Psycho-Oncology, 5, 23–29. https://doi.org/10.1002/(SICI)1099-1611(199603)5:1<23::AID-PON206>3.0.C…
Institute of Medicine. (2008). Cancer care for the whole patient: Meeting psychosocial health needs. Washington, DC: National Academies Press.
Janda, M., Steginga, S., Langbecker, D., Dunn, J., Walker, D., & Eakin, E. (2007). Quality of life among patients with a brain tumor and their carers. Journal of Psychosomatic Research, 63, 617–623. https://doi.org/10.1016/j.jpsychores.2007.06.018
Ji, J., Zöller, B., Sundquist, K., & Sundquist, J. (2012). Increased risks of coronary heart disease and stroke among spousal caregivers of cancer patients. Circulation, 125, 1742–1747. https://doi.org/10.1161/CIRCULATIONAHA.111.057018
Kent, E.E., Rowland, J.H., Northouse, L., Litzelman, K., Chou, W.-Y., Shelburne, N., . . . Huss, K. (2016). Caring for caregivers and patients: Research and clinical priorities for informal cancer caregiving. Cancer, 122, 1987–1995. https://doi.org/10.1002/cncr.29939
Kissane, D.W. (2013). Marriage is as protective as chemotherapy in cancer care. Journal of Clinical Oncology, 31, 3852–3853. https://doi.org/10.1200/JCO.2013.51.5080
Longacre, M., Miller, M., Golant, M., Kennedy, V., Zaleta, A., & Buzaglo, J. (2017). Psychometric properties of a 47-item distress screening tool for caregivers of cancer patients in a community-based sample. Paper presented at the 38th Annual Scientific Session of the Society for Behavorial Medicine, San Diego, CA.
Miles, M.B., Huberman, A.M., & Saldaña, J. (2014). Qualitative data analysis: A methods sourcebook (3rd ed.). Thousand Oaks, CA: Sage.
Miller, M.F., Mullins, C.D., Onukwugha, E., Golant, M., & Buzaglo, J.S. (2014). Discriminatory power of a 25-item distress screening tool: A cross-sectional survey of 251 cancer survivors. Quality of Life Research, 23, 2855–2863. https://doi.org/10.1007/s11136-014-0742-4
Morris, B.A., Thorndike, F.P., Ritterband, L.M., Glozier, N., Dunn, J., & Chambers, S.K. (2015). Sleep disturbance in cancer patients and caregivers who contact telephone-based help services. Supportive Care in Cancer, 23, 1113–1120. https://doi.org/10.1007/s00520-014-2458-y
Morris, S.M., & Thomas, C. (2001). The carer’s place in the cancer situation: Where does the carer stand in the medical setting? European Journal of Cancer Care, 10, 87–95.
National Alliance for Caregiving. (2016). Cancer caregiving in the U.S.: An intense, episodic, and challenging care experience. Retrieved from http://www.caregiving.org/wp-content/uploads/2016/06/CancerCaregivingRe…
National Alliance for Caregiving & AARP Public Policy Institute. (2015). 2015 report: Caregiving in the U.S. Retrieved from https://www.aarp.org/content/dam/aarp/ppi/2015/caregiving-in-the-united…
National Comprehensive Cancer Network. (2018). NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines®): Distress management [v.2.2018]. Retrieved from https://www.nccn.org/professionals/physician_gls/pdf/distress.pdf
Nightingale, C.L., Sterba, K.R., Tooze, J.A., Milliron, B.-J., Tetrick, L.A., Paek, M.-S., & Weaver, K.E. (2016). Vulnerable characteristics and interest in wellness programs among head and neck cancer caregivers. Supportive Care in Cancer, 24, 3437–3445. https://doi.org/10.1007/s00520-016-3160-z
Northouse, L.L., Katapodi, M.C., Song, L., Zhang, L., & Mood, D.W. (2010). Interventions with family caregivers of cancer patients: Meta-analysis of randomized trials. CA: A Cancer Journal for Clinicians, 60, 317–339. https://doi.org/10.3322/caac.20081
Patton, M.Q. (2002). Qualitative research and evaluation methods (3rd ed.). Thousand Oaks, CA: Sage.
Porter, L.S., & Dionne-Odom, J.N. (2017). Supporting cancer family caregivers: How can frontline oncology clinicians help? Cancer, 123, 3212–3215. https://doi.org/10.1002/cncr.30759
Ramirez, A., Addington-Hall, J., & Richards, M. (1998). ABC of palliative care. The carers. BMJ, 316, 208–211.
Shaffer, K.M., Kim, Y., & Carver, C.S. (2016). Physical and mental health trajectories of cancer patients and caregivers across the year post-diagnosis: A dyadic investigation. Psychology and Health, 31, 655–674. https://doi.org/10.1080/08870446.2015.1131826
Shaw, J., Harrison, J., Young, J., Butow, P., Sandroussi, C., Martin, D., & Solomon, M. (2013). Coping with newly diagnosed upper gastrointestinal cancer: A longitudinal qualitative study of family caregivers’ role perception and supportive care needs. Supportive Care in Cancer, 21, 749–756. https://doi.org/10.1007/s00520-012-1575-8
Sklenarova, H., Krümpelmann, A., Haun, M.W., Friederich, H.-C., Huber, J., Thomas, M., . . . Hartmann, M. (2015). When do we need to care about the caregiver? Supportive care needs, anxiety, and depression among informal caregivers of patients with cancer and cancer survivors. Cancer, 121, 1513–1519.
Sobel, D.S. (2000). The cost-effectiveness of mind–body medicine interventions. Progress in Brain Research, 122, 393–412. https://doi.org/10.1016/S0079-6123(08)62153-6
Vanderwerker, L.C., Laff, R.E., Kadan-Lottick, N.S., McColl, S., & Prigerson, H.G. (2005). Psychiatric disorders and mental health service use among caregivers of advanced cancer patients. Journal of Clinical Oncology, 23, 6899–6907.
Vitaliano, P.P., Scanlan, J.M., Zhang, J., Savage, M.V., Hirsch, I.B., & Siegler, I.C. (2002). A path model of chronic stress, the metabolic syndrome, and coronary heart disease. Psychosomatic Medicine, 64, 418–435.
Waldron, E.A., Janke, E.A., Bechtel, C.F., Ramirez, M., & Cohen, A. (2013). A systematic review of psychosocial interventions to improve cancer caregiver quality of life. Psycho-Oncology, 22, 1200–1207. https://doi.org/10.1002/pon.3118
Zaleta, A.K., Longacre, M.L., Miller, M., Golant, M., Kennedy, V., Miller, K., & Buzaglo, J.S. (2017). Refining a validated distress screening tool for caregivers of cancer patients in a community-based sample. Poster presented at the 22nd Annual Conference of the National Comprehensive Cancer Network, Orlando, FL.




