Perceptions of Clinical Trial Participation Among Women of Varying Health Literacy Levels
Purpose: To understand the perceptions of risk, benefit, and the informed consent process after enrolling in and completing a phase 2 clinical trial using intraoperative radiation therapy (IORT) for early-stage breast cancer, and to determine how perceptions varied based on women’s health literacy levels.
Participants & Setting: 20 participants who had already completed a phase 2 IORT clinical trial for early-stage breast cancer at an academic medical center.
Methodologic Approach: A qualitative descriptive study was conducted using structured interviews consisting of questions aimed to elicit responses from participants regarding experiences of informed consent and the research process. A validated brief health literacy questionnaire was used to determine health literacy levels of participants. The authors analyzed themes using inductive thematic analysis.
Findings: Women with lower levels of health literacy reported feeling confident enough in the provider to make the decision to enroll in the clinical trial during the initial consultation, and, in general, women reported relying heavily on provider recommendation for enrolling in the clinical trial.
Implications for Nursing: Tailored approaches for patients with limited health literacy are needed during the clinical trial consent process. Additional longitudinal research with a larger sample size can extend study results and provide insight into the most effective way to modify the informed consent process for patients with limited health literacy.
Jump to a section
Health literacy refers to the ability to comprehend, as well as the ability to obtain, appraise, and integrate, health-related knowledge (Nielsen-Bohlman et al., 2004). A patient’s health literacy level is an important element of high-quality care that can affect decisions and actions of patients and providers. Educational background is not always predictive of health literacy levels; an individual’s health literacy level may be lower than his or her general literacy, meaning that even highly educated adults may have limited health literacy (Davis et al., 2002). An estimated 20%–36% of all adults in the United States have limited health literacy, and the estimate is even higher among low-income individuals (Nielsen-Bohlman et al., 2004). Limited health literacy is associated with limited engagement in health care, including limited access to information, limited social support, increased stigma, and limited involvement in medical decision making (Berkman et al., 2011; Easton et al., 2013; Keim-Malpass et al., 2015; Melhado & Bushy, 2011). Limited health literacy has also been associated with higher use of health care, lower quality of life, and worse outcomes in objective measures of chronic illness control (e.g., higher hemoglobin A1C in those with a history of type 2 diabetes mellitus, worse asthma control) (Berkman et al., 2011; DeWalt et al., 2007; Sørensen et al., 2012).
The impact of health literacy on the oncology population is of particular importance, because cancer care commonly requires patients to navigate a complex healthcare system containing multiple possible specialties, screening recommendations, and treatment options (Keim-Malpass et al., 2017, 2018). Particularly among patients with breast cancer, diagnosis and treatment may involve a number of shared decisions (e.g., deciding between mastectomy and breast-conserving therapy with adjuvant radiation, the decision to enroll in a clinical trial). When faced with a difficult diagnosis, increased emotional stress may increase the time needed to understand and integrate new information (Sudore et al., 2006). This shared decision-making process is made more challenging when limited health literacy is an added factor (Koh et al., 2013).
As clinical trials become more common as treatment options for individuals with cancer, components of the research and informed consent process are often unfamiliar for patients (Tam et al., 2015) and may lead to confusion about voluntary participation, risks and benefits of treatment, freedom to withdraw, and availability of alternative treatment. Despite attempts to write informed consents for clinical trials at a grade school reading level, they are often written at a high school or college reading level because of the complexity of medical terminology and study procedures, which impedes comprehension among patients with limited health literacy (Simonds et al., 2017). Beyond reading level, the informed consent process involves explaining difficult concepts to potential participants. These concepts may include randomization, potential for placebo, and clinical equipoise, or the concept that investigators hypothesize that the therapeutic being tested is superior to standard therapy, but they are unsure. Finally, there are many elements that make clinical trial decisions difficult among those with a diagnosis of cancer, including other cultural factors that may influence a person’s understanding of clinical trial participation (Asiedu et al., 2018; Kao et al., 2018).
Previous research has assessed the relationship between limited health literacy and patient comprehension of consent forms, but this research was based on hypothetical clinical trials and not trials that participants were actually considering (Livaudais-Toman et al., 2014). Alternatively, Krieger et al. (2016) concluded that those with high health literacy expressed less intent to enroll in a clinical trial because of the perception that clinical trials are not individualized treatment options. Although not explicitly measured, the authors concluded that this was likely because of the notion that those with high levels of health literacy could appraise information from a variety of sources and more easily integrate diverse information types into their own decision-making strategy (Krieger et al., 2016).
To date, the available research indicates that tailored informed consent processes are needed for individuals with limited health literacy, but the relationship between health literacy and understanding of risks and benefits of clinical trial enrollment have not yet been established. The purpose of this qualitative study was to assess the perceptions of risks, benefits, and the informed consent process for patients who were already enrolled in a phase 2 clinical trial using intraoperative radiation therapy (IORT). The focus of the nested qualitative study was to explore how the perceptions of risks and benefits of clinical trial enrollment differed based on varying levels of health literacy.
Methods
Sample and Parent Study
Following University of Virginia Institutional Review Board approval, this study used a cross-sectional qualitative description design (Sandelowski, 2000). A convenience sample of 50 potential participants consisting of women aged 45–90 years was called to seek consent for the nested qualitative study from November 2017 through March 2018. Study participants were included in the qualitative study if they were already enrolled in and completed a phase 2 clinical trial and had also completed their three-month follow-up visit after initial treatment. The purpose of this parent study was to determine the efficacy of single-fraction precision breast IORT using a multi-lumen balloon applicator and in-room computed tomography imaging for the treatment of early-stage breast cancer (Trifiletti et al., 2015). In the parent study, a total fraction of 12.5 Gy radiation was delivered to each patient in one dose at the time of lumpectomy, whereas traditional radiation treatments involve a cumulative dose of around 45 Gy of radiation delivered five days a week for four to six weeks. Preliminary safety data regarding IORT have been established, but long-term follow-up data, including rates of recurrence, have not yet been well-defined (Trifiletti et al., 2015). This phase 2 trial is an optimal parent study for qualitative follow-up because the decision to participate requires a nuanced understanding of individual risk and benefit.
Data Collection and Analysis
Eligible participants were recruited directly via telephone. Verbal consent was obtained over the telephone, and the consented study participant arranged a convenient time for a 30-minute interview. At the time of the interview, a script was followed to ensure consistency across interviews and to minimize bias (see Figure 1). Interviews were audio recorded and then transcribed verbatim. Field notes were also maintained to document perceptions and context of each interview. 
The Set of Brief Screening Questions (SBSQ), a validated health literacy screening questionnaire, was used to determine each participant’s health literacy score. The SBSQ is a three-item self-report health literacy assessment that was developed for researchers and clinicians to access an adequate screening measure with low patient burden (Sarkar et al., 2011). The three items are as follows:
• How confident are you in filling out medical forms? (1 = extremely, 2 = quite a bit, 3 = somewhat, 4 = a little, 5 = not at all)
• How often do you have problems learning about your medical condition because of difficulty understanding written information? (1 = never, 2 = rarely, 3 = sometimes, 4 = often, 5 = always)
• How often do you have someone help you read hospital materials? (1 = never, 2 = rarely, 3 = sometimes, 4 = often, 5 = always)
Scores range from 3–15, with higher scores representing lower self-reported health literacy. The SBSQ has been validated against the Test of Functional Health Literacy in Adults, the gold standard in health literacy assessment among adults, and has been determined to be able to distinguish English and Spanish speakers with adequate health literacy (5 or lower) from those with marginal health literacy (6–7) and inadequate health literacy (8–15) (Sarkar et al., 2011). Health literacy scores for each participant were recorded and maintained in the patient electronic health record as a part of a quality initiative project focused on health literacy (Keim-Malpass et al., 2017, 2018).
Qualitative descriptive analysis was used for analysis and interpretation of qualitative data collected during the participant interviews (Sandelowski, 2010). The textual data from the transcriptions of the interviews and field notes were analyzed via line-by-line analysis, and reduction of the textual data was done through inductive open coding and constant comparative analysis (Creswell, 1998). After line-by-line analysis of the transcripts, nodes were grouped together to form inductive themes. Trustworthiness was addressed by making all aspects of the study design open for review by the members of the research team, allowing for open peer review for decisions made as a part of the audit trail, and having all team members review thematic content (Lincoln & Guba, 1985).
Results
The final convenience sample consisted of 20 women who had undergone the phase 2 precision IORT clinical trial. Of the 20 study participants, 16 were in the 24-month follow-up window from the parent study and 4 were in the 18-month follow-up window. Six participants enrolled were of limited or marginal health literacy levels (score of 6 or higher on the health literacy screening questionnaire). Table 1 summarizes participant characteristics for this study. The mean age of the women in this study was 67.8 years (SD = 6.99). The mean health literacy level of the participants enrolled in the trial was 4.7 (SD = 8.01). The mean health literacy level of the participants called and not consented in the qualitative study (either because of lack of response or declining consent) was 5.1 (representing lower health literacy). Several themes were identified, including weights of risks and benefits, pragmatic decision making, and confidence in provider recommendation. 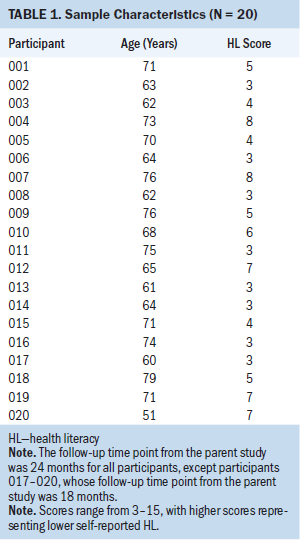
Weight of Risks and Benefits
Participants were asked what risks and benefits they remembered as part of the informed consent process of the parent study. Responses included not remembering any risks to self, the benefit of having a single radiation treatment, and the benefit of having a larger team of providers caring for them.
Of the 20 participants interviewed, 8 answered that they did not believe there were any risks of enrolling in the trial. Responses included not seeing any direct risks to self (“I didn’t see any great risk” [participant 009, health literacy score of 5, adequate health literacy]), as well as feeling that they were not told of any risks at all (“I wasn’t told of any risks, actually” [participant 002, health literacy score of 3, adequate health literacy]). Five participants responded to this question by recalling that the main risk was that, because this was a clinical trial, this version of treatment may not completely eradicate the cancer and they may have to undergo additional treatment. (For context, this would be if there was failure to achieve adequate clear margins in the initial surgery and IORT treatment, the recommendation would be to complete a traditional course of external-beam radiation). Responses included statements such as, “The cons were, you know, you’re part of a study and there’s no guarantee” (participant 003, health literacy score of 3, adequate health literacy), and “The risk would be that it wouldn’t get, you know, taken care of. . . . It might have been worse” (participant 017, health literacy score of 3, adequate health literacy).
Participants focused on the benefits of participating in this trial, with the most common response being that, by participating in the parent study, their course of treatment would be shorter than if they underwent traditional radiation treatment. Participants noted the convenience of the study treatment as an influential factor in their decision, stating, “It still beat the four weeks, five days a week treatment, so I thought it was very convenient” (participant 019, health literacy score of 7, marginal health literacy), and “I liked it because I qualified for it because it was a one-dose radiation, convenient” (participant 002, health literacy score of 3, adequate health literacy). Sixteen participants said that this was the main reason they decided to enroll in the trial.
Seven participants spoke of a benefit of having a larger team of people working with them by enrolling in the clinical trial. One participant claimed this as a benefit by stating,
The benefits were, you know, that everybody was on top of it, constantly. . . . I felt like I was, you know, so monitored so well and that if anything did come up, you know, that they would take care of it. (participant 006, health literacy score of 3, adequate health literacy)
Another stated, “I felt like I had an extra pair of eyes of what was going on because . . . I was participating in a study” (participant 005, health literacy score of 4, adequate health literacy).
Participants stated that a perceived benefit of clinical trial participation was that, in addition to their regular team of practitioners who would be monitoring them for problems or signs of recurrence after the trial ended, additional clinicians would be involved in their care. Although this appeared as a benefit to seven participants, one spoke of this as a risk or frustration with the clinical trial because of the number of people who were in the room at appointments, recalling that “it’s a difficult time anyway, and the last thing you need is . . . 5,000 people looking at you, poking at you, and I just did not think that was a good idea” (participant 002, health literacy score of 3, adequate health literacy).
Pragmatic Decision Making
When asked about the difficulty of the decision to enroll in the clinical trial, 17 participants said that it was an easy decision to make. This was largely because of how they gathered information and came to their conclusions. Before enrolling, participants gathered more information from their surgeons, their friends and family, and the Internet to feel more confident in their decision.
Ten participants stated that they spoke with friends and family members prior to enrolling in the trial, and six spoke specifically with family members or friends who had undergone whole-breast radiation for treatment of cancer. Of the participants who had spoken with people who had personal histories of cancer and had undergone traditional treatment measures, all stated that this influenced their decision and gave them more confidence in enrolling in the clinical trial. One participant recalled feeling reluctant to enroll in the trial prior to receiving input from friends and spoke of how this affected her decision:
I was a little reluctant because I really didn’t know that much about the IORT at first. But then I talked, actually after talking to a friend of mine who had, you know, the traditional radiation, she said, “Man, I can’t imagine how much better it would be just to do it once, just to have one dose of radiation.” . . . So after talking to my friend who had a very bad experience, she got burned. . . . I just decided I didn’t want to do the traditional. (participant 013, health literacy score of 3, adequate health literacy)
Eight participants stated that they used the Internet to find more information prior to enrolling in the trial. These participants responded that they looked up more information about their cancer, treatment options, and outcomes after their initial diagnosis, which helped them feel more informed. The process of researching more information online helped participants feel more confident in their decision because they were more aware of all of their options and felt they knew all of the facts. One participant spoke of her own research:
I did a lot of research on my own just trying to research, you know, some medical papers on the use of this, whatever they call the radiation. . . . I just tried to read as much as I could and ask as many questions as I could at [Dr. X]. (participant 008, health literacy score of 3, adequate health literacy)
Confidence in Provider Recommendation
The experience of working with the healthcare providers affected the decision to enroll in the trial for 18 participants, with these participants stating that the confidence they felt in their providers made them more comfortable with the clinical trial as a treatment option. How confidence in providers affected this decision is evident in the following:
Oh, I felt [the physician] and the people that work with her were very good at explaining the trial to come and what the procedure entailed, and they were very thorough in preparing me mentally for it, and I just felt very well informed and secure in their talents. (participant 003, health literacy score of 4, adequate health literacy)
This finding was also true of participants who had limited health literacy, including common mentions of thorough preparation and understanding, as well as confidence in staff abilities:
It was extremely thorough and there was a lot of printed material, a workbook that I took home with me, and I felt that I understood fairly well by their descriptions of everything, so I was very pleased. [It influenced my decision to enroll in the trial] because I felt that they were competent. (participant 010, health literacy score of 6, marginal health literacy)
Another participant said,
I was concerned and I was very open, and they were open with me in explaining what the procedure would be. . . . I almost made it right there on the spot because I just felt so secure that my problem would be taken care of. (participant 019, health literacy score of 7, marginal health literacy)
Five participants claimed that they were able to make their decision during their initial consultation without seeking further information. One participant recalled:
The only person I went to was Dr. [X], who was my surgeon. . . . I just went by the recommendation, I believe the choices I had from my doctor. I had two choices here, and I decided to choose the one that was least cumbersome, put it that way. (participant 007, health literacy score of 8, inadequate health literacy)
The other four participants shared similar experiences of feeling confident in their decision because of their confidence in their provider to the point of not needing additional information or consultation when deciding to enroll in the trial.
Discussion
This study highlights the process of clinical trial decision making among women with varying levels of health literacy by weighing the risks and benefits, thinking pragmatically about whether to enroll or undergo traditional radiation, and having confidence in providers. The belief of a lack of risks associated with this treatment option was described in conjunction with greater confidence in making the decision to enroll. Participants who remembered recurrence as a risk of enrolling in the trial had an average health literacy score of 4, which is indicative of having higher health literacy than the average of the entire sample. Participants’ understanding of the risk of recurrence, as well as the weight of this risk in the decision-making process, could be related to having a greater comprehension of the consent. Additional research is needed among a larger sample population to determine the significance of understanding the risks and benefits in the enrollment process for clinical trials.
Seeking out additional information and conducting personal research on the Internet helped some participants feel more informed and confident in their decision. Participants who used other resources, such as the Internet, in their decision had, on average, higher health literacy scores compared to the entire sample, although no statistical difference existed between the two groups. These results are consistent with the definition of health literacy as the ability to obtain, appraise, and integrate health-related knowledge, as higher health literacy levels could be associated with greater research into treatment options because of greater access to information, the knowledge to understand what to look for, an understanding of personal knowledge gaps, and the knowledge of what information was pertinent to their diagnosis and treatment (Koh et al., 2013; Morris et al., 2013). Higher levels of health literacy are associated with greater comprehension (Coyne et al., 2003; Davis et al., 1998; Krieger et al., 2016; Sudore et al., 2006), and the results of this study show that higher health literacy could also be associated with greater research, questioning, and likelihood to seek out additional information prior to making decisions related to healthcare treatment plans. Additional study with a larger sample size is needed to confirm these results.
Relationships with providers influenced the decision-making process for the majority of participants, with 90% of participants claiming that having confidence in their surgeons made them feel confident in making the decision to enroll in the clinical trial. Some participants felt so confident in their provider that they did not see a necessity in seeking out any more information or doing any further research prior to making their decision. This finding could be related to absolute trust in their provider, as well as a desire for the provider to make the decision for them. Patients with limited health literacy may not have the ability to determine what more they may need to know when making decisions related to their health or the extent of the treatment options and plans.
Limitations
The results of this study may not be generalizable for all clinical trials because only participants who had already enrolled in the parent study were included. A potential for bias in the data exists because of the inclusion and exclusion criteria that required participants to have already completed their treatment in the parent study. The experiences of the consent process could be clouded by their experiences within the trial as a whole or their experiences with their current state of health after treatment completion. Because the participants were all greater than 18 months postoperative from their treatment in the parent study, an increased chance of biased data exists because of risk of forgetfulness or altered perceptions of the consent process based on the amount of time that has elapsed. A larger sample size is needed among a more diverse sample of varying ages and cancer diagnoses to make the results generalizable to all clinical trials.
Implications for Nursing
Based on the results of this study, health literacy levels may influence the decision-making process by affecting how well patients comprehend treatment risks and benefits, and how they use and seek out information that affects their treatment decisions. Because patients with limited health literacy may be less likely to seek out additional health information on their own, clinicians must be sure to offer tailored approaches to translating the risks and benefits of clinical trials. Greater comprehension has been shown to be associated with lower levels of anxiety (Davis et al., 1998; Evans et al., 2011). Clinicians must also understand that a lack of questions from a patient does not necessarily indicate comprehension, because participants who asked the most questions and did more information appraisal had the highest levels of health literacy.
This study has important implications for oncology nurses because nurses are often involved in the shared decision-making and informed consent process for clinical trials. Oncology nurses have a unique opportunity to initiate patient-centered consultation that is inclusive of the patient’s health literacy. Obtaining the patient’s health literacy score should be the standard of care for every patient in oncology as a quality measure and can be obtained quickly and integrated into clinic workflow (Keim-Malpass et al., 2017). 
Conclusion
This study highlights the need for alternative representations of clinical trial risks and benefits beyond written materials and patient consultation. Further research must be done to determine the best way to tailor the consent process to the needs of all individuals with cancer, focusing on presenting information in a comprehensive and easy-to-read manner. The authors recommend that oncology nurses take a participatory family-centered approach during clinical trial consultation so those with limited health literacy are not solely reliant on provider recommendation. 
About the Author(s)
Allison C. Burks, BSN, RN, is an RN in the Duke University Health System in Chapel Hill, NC; and Aubrey Doede, MSN, RN, is a PhD student in the School of Nursing, Shayna L. Showalter, MD, is an associate professor of surgery in the School of Medicine, and Jessica Keim-Malpass, PhD, RN, is an assistant professor in the School of Nursing, all at the University of Virginia in Charlottesville. This work was supported by an internal University of Virginia Women’s 4 Miler Breast Care grant. Burks, Showalter, and Keim-Malpass completed the conceptualization and design. Burks completed the data collection. Burks and Keim-Malpass provided statistical support and analysis. All authors contributed to the manuscript preparation. Keim-Malpass can be reached at jlk2t@virginia.edu, with copy to ONFEditor@ons.org. (Submitted June 2019. Accepted December 6, 2019.)
References
Asiedu, G.B., Ridgeway, J.L., Carroll, K., Jatoi, A., & Radecki Breitkopf, C. (2018). “Ultimately, mom has the call”: Viewing clinical trial decision making among patients with ovarian cancer through the lens of relational autonomy. Health Expectations, 21(6), 981–989. https://doi.org/10.1111/hex.12691
Berkman, N.D., Sheridan, S.L., Donahue, K.E., Halpern, D.J., Viera, A., Crotty, K., . . . Viswanathan, M. (2011). Health literacy interventions and outcomes: An updated systematic review (Evidence Report/Technology Assessment 199, AHRQ Publication Number 11-E006). Agency for Healthcare Research and Quality. https://www.ahrq.gov/downloads/pub/evidence/pdf/literacy/literacyup.pdf
Coyne, C.A., Xu, R., Raich, P., Plomer, K., Dignan, M., Wenzel, L.B., . . . Cella, D. (2003). Randomized, controlled trial of an easy-to-read informed consent statement for clinical trial participation: A study of the Eastern Cooperative Oncology Group. Journal of Clinical Oncology, 21(5), 836–842. https://doi.org/10.1200/jco.2003.07.022
Creswell, J.W. (1998). Qualitative inquiry and research design: Choosing among five traditions (1st ed.). Sage.
Davis, T.C., Berkel, H.J., Holcombe, R.F., Pramanik, S., & Divers, S.G. (1998). Informed consent for clinical trials: A comparative study of standard versus simplified forms. Journal of the National Cancer Institute, 90(9), 668–674. https://doi.org/10.1093/jnci/90.9.668
Davis, T.C., Williams, M.V., Marin, E., Parker, R.M., & Glass, J. (2002). Health literacy and cancer communication. CA: A Cancer Journal for Clinicians, 52(3), 134–149. https://doi.org/10.3322/canjclin.52.3.134
DeWalt, D.A., Dilling, M.H., Rosenthal, M.S., & Pignone, M.P. (2007). Low parental literacy is associated with worse asthma care measures in children. Ambulatory Pediatrics, 7(1), 25–31. https://doi.org/10.1016/j.ambp.2006.10.001
Easton, P., Entwistle, V.A., & Williams, B. (2013). How the stigma of low literacy can impair patient-professional spoken interactions and affect health: Insights from a qualitative investigation. BMC Health Services Research, 13, 319. https://doi.org/10.1186/1472-6963-13-319
Evans, K.R., Lewis, M.J., & Hudson, S.V. (2011). The role of health literacy on African American and Hispanic/Latino perspectives on cancer clinical trials. Journal of Cancer Education, 27(2). https://doi.org/10.1007/s13187-011-0300-5
Kao, C.Y., Aranda, S., Krishnasamy, M., & Hamilton, B. (2018). Identifying essential information to support patient decision-making regarding participation in cancer clinical trials: A Delphi study. European Journal of Cancer Care, 27(6), e12954. https://doi.org/10.1111/ecc.12954
Keim-Malpass, J., Doede, A., Camacho, F., Kennedy, C., & Showalter, S.L. (2018). Impact of patient health literacy on surgical treatment of breast cancer. Breast Journal, 24(4), 633–636. https://doi.org/10.1111/tbj.13011
Keim-Malpass, J., Doede, A., Kennedy, C., & Showalter, S. (2017). Health literacy assessment: Feasibility in a breast surgical oncology clinic. Clinical Journal of Nursing Oncology, 21(3), 384–386. https://doi.org/10.1188/17.cjon.384-386
Keim-Malpass, J., Letzkus, L.C., & Kennedy, C. (2015). Parent/caregiver health literacy among children with special health care needs: A systematic review of the literature. BMC Pediatrics, 15(1), 92. https://doi.org/10.1186/s12887-015-0412-x
Koh, H.K., Brach, C., Harris, L.M., & Parchman, M.L. (2013). A proposed ‘health literate care model’ would constitute a systems approach to improving patients’ engagement in care. Health Affairs, 32(2), 357–367.
Krieger, J.L., Neil, J.M., Strekalova, Y.A., & Sarge, M.A. (2016). Linguistic strategies for improving informed consent in clinical trials among low health literacy patients. Journal of the National Cancer Institute, 109(3), djw233. https://doi.org/10.1093/jnci/djw233
Lincoln, Y., & Guba, E. (1985). Naturalistic inquiry. Sage.
Livaudais-Toman, J., Burke, N.J., Napoles, A., & Kaplan, C.P. (2014). Health literate organizations: Are clinical trial sites equipped to recruit minority and limited health literacy patients? Journal of Health Disparities Research and Practice, 7(4), 1–13.
Melhado, L., & Bushy, A. (2011). Exploring uncertainty in advance care planning in African Americans: Does low health literacy influence decision making preference at end of life. American Journal of Hospice and Palliative Medicine, 28(7), 495–500. https://doi.org/10.1177/1049909110398005
Morris, N.S., Field, T.S., Wagner, J.L., Cutrona, S.L., Roblin, D.W., Gaglio, B., . . . Mazor, K.M. (2013). The association between health literacy and cancer-related attitudes, behaviors, and knowledge. Journal of Health Communication, 18(Suppl. 1), 223–241. https://doi.org/10.1080/10810730.2013.825667
Nielsen-Bohlman, L., Panzer, A.M., & Kindig, D.A. (Eds.). (2004). Health literacy: A prescription to end confusion. National Academies Press. https://doi.org/10.17226/10883
Sandelowski, M. (2010). What’s in a name? Qualitative description revisited. Research in Nursing and Health, 33(1), 77–84.
Sarkar, U., Schillinger, D., López, A., & Sudore, R. (2011) Validation of self-reported health literacy questions among diverse English and Spanish-speaking populations. Journal of General Internal Medicine, 26(3), 265–271. https://doi.org/10.1007/s11606-010-1552-1
Simonds, V.W., Garroutte, E.M., & Buchwald, D. (2017). Health literacy and informed consent materials: Designed for documentation, not comprehension of health research. Journal of Health Communication, 22(8), 682–691. https://doi.org/10.1080/10810730.2017.1341565
Sørensen, K., Van den Broucke, S., Fullam, J., Doyle, G., Pelikan, J., Slonska, Z., & Brand, H. (2012). Health literacy and public health: A systematic review and integration of definitions and models. BMC Public Health, 12, 80. https://doi.org/10.1186/1471-2458-12-80
Sudore, R.L., Landefeld, C.S., Williams, B.A., Barnes, D.E., Lindquist, K., & Schillinger, D. (2006). Use of a modified informed consent process among vulnerable patients: A descriptive study. Journal of General Internal Medicine, 21(8), 867–873. https://doi.org/10.1111/j.1525-1497.2006.00535.x
Tam, N., Huy, N., Thoa, L., Long, N., Trang, N., Hirayama, K., & Karbwang, J. (2015). Participants’ understanding of informed consent in clinical trials over three decades: Systematic review and meta-analysis. Bulletin of the World Health Organization, 93(3), 1. https://doi.org/10.2471/BLT.14.141390
Trifiletti, D.M., Showalter, T.N., Libby, B., Brenin, D.R., Schroen, A.T., Reardon, K.A., & Showalter, S.L. (2015). Intraoperative breast radiation therapy with image guidance: Findings from CT images obtained in a prospective trial of intraoperative high-dose-rate brachytherapy with CT on rails. Brachytherapy, 14(6), 919–924. https://doi.org/10.1016/j.brachy.2015.07.001




